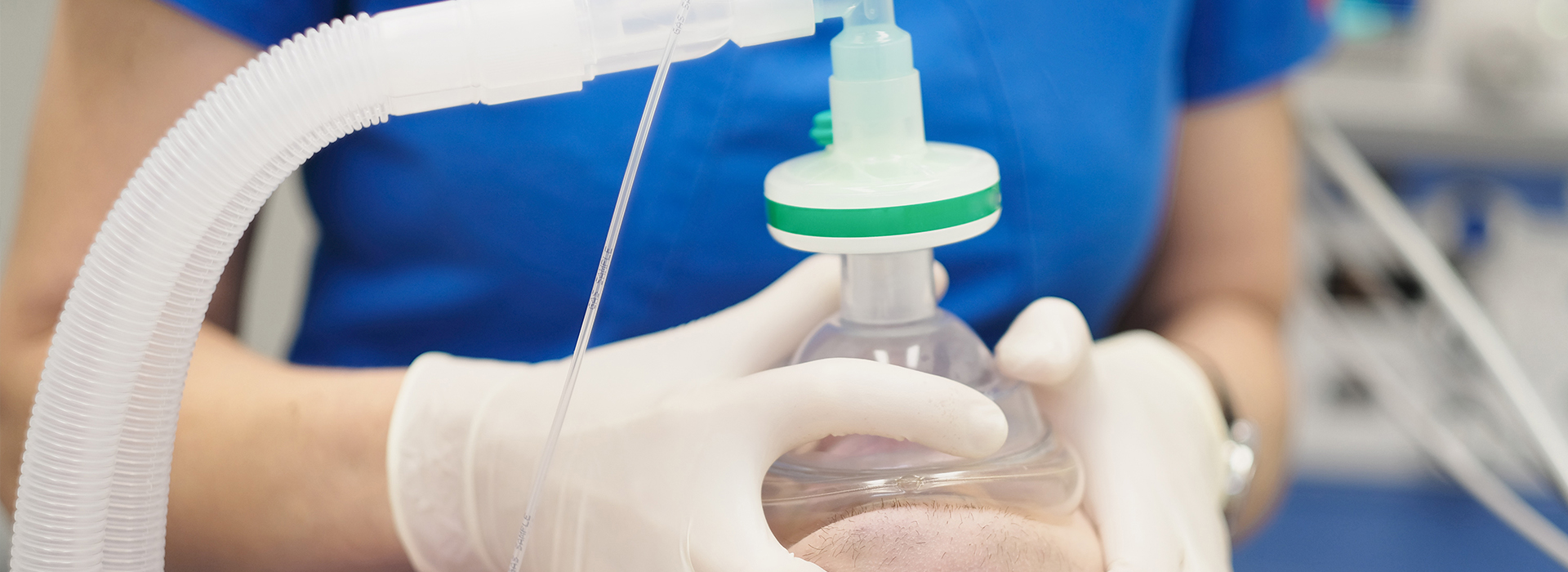
Dental fear is common — many people put off or avoid dental visits because the idea of treatment causes real stress. If anxiety keeps you from getting the care you need, the office of Granby Dental Center offers respectful, evidence-based sedation options to help patients feel calm and cooperative during appointments. Our goal is to remove the emotional barriers that stand between you and maintaining healthy teeth and gums.
Skipping regular care can allow small problems to grow into larger ones. Sedation dentistry is a tool that lets anxious or sensitive patients receive thorough treatment with dignity and minimal discomfort. When used appropriately, sedation reduces the tension and memory of a procedure, making it possible to complete the dental work you need in a single visit or with fewer appointments.
We take a thoughtful approach to sedation: matching the level of medication to the procedure and the patient’s medical history so every visit is safe, controlled, and as comfortable as possible. Read on to learn how sedation can help, what options are available, and what to expect before, during, and after treatment.
Dental sedation works by reducing the body’s stress response and promoting a sense of calm. For many patients, this means they can sit through treatment without the adrenaline, muscle tension, or panic that otherwise makes care impossible. Sedation does not remove the dentist’s ability to communicate with the patient in most cases — instead it creates a relaxed state where instructions are followed easily and without distress.
Beyond immediate comfort, sedation often improves overall treatment outcomes. When a patient is relaxed, the clinician can work more efficiently and precisely, which can shorten appointment time and reduce the need for repeated visits. This is especially helpful when multiple procedures or complex restorations are required.
Importantly, sedation is not a one-size-fits-all solution. The right approach depends on a patient’s health background, medication sensitivities, level of anxiety, and the nature of the dental work. Our team discusses options openly and tailors a plan so patients feel informed and in control of their care.
People choose sedation for many reasons. For some, a long-standing dental phobia prevents routine checkups entirely; for others, a particular procedure — such as extracting a tooth or placing implants — triggers intense nervousness. Sedation bridges that gap, allowing these patients to receive timely treatment rather than deferring care.
Sedation is also useful for people who have a strong gag reflex, hypersensitive teeth, or difficulty keeping still for extended periods. Pediatric patients, adults with special healthcare needs, and anyone with limited tolerance for dental instruments can benefit from an individualized sedation plan that increases comfort and cooperation.
When extensive treatment is needed, sedation can make it practical to complete more work in a single appointment. That reduces the overall number of visits and the cumulative stress of repeated procedures, letting patients restore oral health with fewer interruptions to their daily lives.
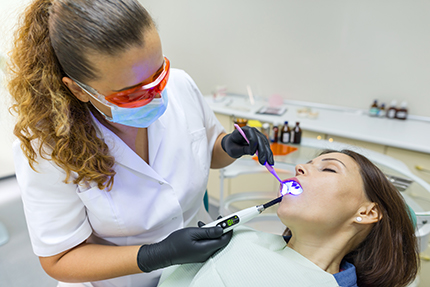
There are several types of sedation used in dental offices, each providing a different depth of relaxation. Our team evaluates your medical history, current medications, and treatment needs when recommending a method. The most common in-office options include inhaled nitrous oxide, prescribed oral medication, and intravenous (IV) sedation.
Selecting the right option is a balance between the level of anxiety to be managed and the complexity of the procedure. Mild sedation might be sufficient for routine restorative work, while deeper but controlled sedation can be appropriate for longer surgical procedures or patients with severe apprehension.
No matter which method is chosen, patient safety is the priority. Trained clinicians monitor vital signs and readiness to ensure the chosen sedation level is both effective and appropriate for the individual.
Conscious sedation describes techniques that relax patients while preserving the ability to respond to verbal cues; breathing remains unassisted and protective reflexes are largely intact. This allows dental teams to provide treatment in a familiar office setting with a strong safety profile for most people.
General anesthesia, by contrast, renders a patient unconscious and is typically administered in a hospital or surgical center by an anesthesiologist. In-office dental practices most often rely on conscious sedation because it provides comfort without the increased risks and logistics of full general anesthesia.
Conscious sedation can be delivered in different ways, and the choice depends on how much sedation is needed and how the patient responds to medications. We review medical conditions, allergies, and prior experiences with sedatives to recommend a plan that achieves a calm, cooperative state without unnecessary depth of sedation.
Monitoring and the ability to adjust doses during a procedure help keep the experience safe and predictable. Patients are always briefed on what to expect so they feel prepared and reassured before arriving for their appointment.
Nitrous oxide, sometimes called laughing gas, is a quick-acting and easily reversible sedative inhaled through a small nasal mask. It calms nerves, reduces sensitivity to stimuli, and fades quickly after the mask is removed, allowing patients to leave the office without a lengthy recovery period.
This option is often ideal for patients with mild to moderate anxiety, those who need a gentle boost of relaxation, or individuals who want to remain quickly alert after their visit. It’s also effective for decreasing gag reflex in sensitive patients.
Oral sedation involves taking a prescribed medication before the appointment that helps the patient arrive in a relaxed state. The medication’s effect varies, from light relaxation to a deeper state in which memory of the procedure is reduced.
Patients receiving oral sedatives typically need a responsible adult to accompany them to and from the appointment, as the effects can linger and make driving unsafe immediately after treatment.
IV sedation delivers medication directly into the bloodstream for precise and rapid control of the sedation level. This approach is suited to patients who require a higher degree of comfort or who need longer procedures completed in a single session.
Because IV sedation is more profound, patients must follow pre-appointment instructions about not eating or drinking and have a trusted escort for the trip home. Continuous monitoring during the visit ensures the patient remains safe and stable throughout treatment.
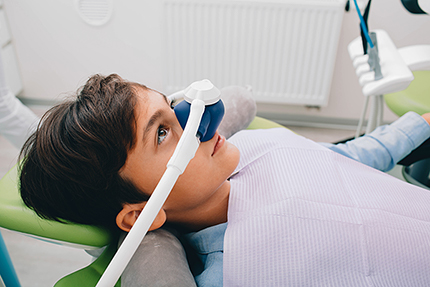
Good sedation starts with clear communication. Be prepared to share your full medical history, current medications (including over-the-counter and herbal supplements), past reactions to anesthesia or sedatives, and any chronic conditions. This information helps clinicians choose the safest sedation route and dose.
Pre-procedure instructions may include fasting for certain sedation types, pausing specific medications, or arranging transportation home. Our team will provide practical, easy-to-follow guidance so you know exactly how to prepare and what to expect on the day of treatment.
Monitoring during and after the procedure — including heart rate, oxygen levels, and responsiveness — is standard practice. Staff members trained in sedation protocols remain with you from induction through recovery, ensuring a controlled environment and a smooth transition back to normal activity.
Recovery depends on the sedation method used. Nitrous oxide wears off quickly and patients often resume normal activities shortly after leaving the office. Oral and IV sedatives may require a longer recovery window; you should plan for rest and avoid activities that demand full attention, like driving, until a clinician confirms it is safe.
Aftercare instructions are tailored to the procedure performed and the sedation used. These can include recommendations for pain management, diet, and signs to watch for that would warrant contacting the dental team. Follow-up appointments are scheduled as needed to check healing and address any questions.
Our clinicians are available to walk you through the entire process — from initial consultation to post-procedure care — so you feel confident every step of the way. Granby Dental Center is committed to providing compassionate, patient-centered sedation services that prioritize safety and comfort.
In summary, sedation dentistry can transform an anxious visit into a manageable, even positive experience. By selecting the appropriate method and following clear safety practices, many patients regain access to essential dental care without fear. Contact us for more information about how sedation could fit into your treatment plan and to discuss which option might be right for you.

Sedation dentistry uses medications to reduce anxiety and increase comfort during dental care. It ranges from mild relaxation to deeper states of calm that still allow the patient to respond to verbal cues. For many people, sedation makes it possible to complete necessary treatments that would otherwise be avoided because of fear or sensitivity. This approach helps patients receive care with dignity and less emotional stress.
Beyond easing anxiety, sedation often improves the efficiency and precision of treatment by helping patients remain still and cooperative. That can shorten appointment time and reduce the number of visits required for complex procedures. Clinicians can work more predictably when a patient is relaxed, which supports better outcomes. Sedation is selected to match both the procedure and the individual patient.
Dental offices commonly offer inhaled nitrous oxide, prescribed oral sedatives, and intravenous (IV) sedation for in-office use. Nitrous oxide acts quickly and wears off soon after the mask is removed, while oral medication is taken before the appointment and may produce a longer-lasting calming effect. IV sedation delivers medication directly into the bloodstream for precise control and is used when deeper relaxation is needed. Each method provides a different depth of sedation and a different recovery profile.
The choice among these options depends on the level of anxiety, the length and complexity of the procedure, and the patient’s medical history. Conscious sedation techniques are designed to maintain protective reflexes and the ability to follow simple commands in most cases. General anesthesia, which renders a patient fully unconscious, is typically provided in a hospital or surgical center and is not the usual in-office approach. Your dental team will explain the benefits and limitations of each method during the consultation.
Most in-office dental sedation falls under the category of conscious sedation, which relaxes patients while preserving the ability to respond to verbal instructions. Under conscious sedation, breathing remains unassisted and protective reflexes are largely intact, allowing the dental team to communicate with and monitor the patient. Patients often feel drowsy and may have limited memory of the procedure, but they are not fully unconscious like they would be under general anesthesia. This balance makes conscious sedation practical and safe for many office-based treatments.
Deeper levels of sedation administered intravenously can produce a greater degree of unawareness for some patients, yet monitoring and trained staff maintain safety throughout the visit. If full unconsciousness is required for complex surgical care, care is typically arranged in a facility equipped for general anesthesia. Your clinician will discuss the expected level of awareness and the reasons for selecting a given sedation approach before treatment begins.
Choosing the appropriate sedation method begins with a thorough review of your medical history, current medications, allergies, and prior experiences with sedatives or anesthesia. The dentist will also consider the level of anxiety, the specific procedure planned, and how long the appointment is expected to last. This information helps match the sedation depth to both safety and comfort needs. Open communication and accurate medical disclosure are essential to making a safe recommendation.
The dental team may adjust the plan based on factors such as respiratory or cardiovascular conditions, interactions with prescription or over-the-counter medications, and any pregnancy or recovery concerns. Monitoring capabilities in the office and the need for post-procedure observation also influence the choice. Your clinician will explain the rationale for the selected option and what preparations and follow-up will be required.
Sedation dentistry is safe when provided by trained professionals following established protocols, including pre-procedure evaluation and continuous monitoring during treatment. Standard monitoring typically includes heart rate, blood pressure, oxygen saturation, and level of responsiveness to ensure the patient remains stable. Staff trained in sedation and emergency procedures remain present from induction through recovery. Safety precautions and readiness to respond to changes are core components of every sedation plan.
Offices that offer sedation follow guidelines for dosing, fasting, and post-procedure care to reduce risk and promote predictable recovery. The chosen sedation level is matched to the patient’s health and the complexity of the procedure, and doses are adjusted as needed during the visit. Patients are briefed on warning signs and aftercare to ensure any concerns are addressed promptly. Clear communication and adherence to safety protocols are key to a successful sedation experience.
Preparation instructions vary by sedation type, but common steps include providing a complete medical history, listing all medications and supplements, and following fasting guidelines if required. Patients receiving oral or IV sedatives are typically advised to arrange a responsible adult to drive them home and remain available after the appointment. Wearing comfortable clothing and avoiding alcohol or recreational substances before the visit helps reduce complications. Your dental team will supply specific, easy-to-follow instructions tailored to your chosen sedation method.
Some medications may need to be paused or adjusted under medical supervision before sedation, so it is important to coordinate with both your dental team and any prescribing physicians when necessary. Inform the office about recent illnesses, changes in health, or pregnancy. Adhering to these preparations improves safety and recovery and ensures the appointed sedation level is appropriate. If you have questions about fasting or medication adjustments, contact the dental office well in advance of your visit.
During induction of sedation you’ll experience a gradual onset of relaxation; nitrous oxide works quickly while oral or IV medications may take longer to reach full effect. The dental team will continuously monitor vital signs and responsiveness and provide local anesthesia as needed for pain control. Communication is usually maintained in a relaxed manner so instructions can be given when necessary. The goal is to keep you comfortable while the clinician completes the planned treatment efficiently.
After the procedure, recovery time depends on the sedation used: nitrous oxide wears off almost immediately, while oral and IV sedatives may require a longer observation and rest period. You should expect some drowsiness and cognitive slowing for several hours following deeper sedation and should avoid driving or operating heavy machinery until cleared by the clinician. Post-procedure instructions regarding pain control, diet, and signs of concern will be provided before you leave, and follow-up appointments are scheduled as needed to monitor healing.
Sedation dentistry can benefit patients with significant dental anxiety, a severe gag reflex, hypersensitive teeth, or limited tolerance for prolonged dental procedures. It is also helpful for people who require extensive restorative work, those with special healthcare needs, and individuals who have had traumatic dental experiences that make routine care difficult. Age alone is not an exclusion, but the chosen sedation method and dosing are adjusted for children and older adults. A candid conversation about health history and treatment goals helps determine candidacy.
Certain medical conditions, medication interactions, or pregnancy may require special consideration or alternative approaches, so candidacy is evaluated on an individual basis. The dental team will assess risks and benefits and coordinate with other healthcare providers when necessary to ensure safety. If sedation is not recommended, the clinician will discuss other strategies to manage anxiety and facilitate comfortable care. The objective is to find the safest, most effective way to complete necessary treatment.
Common, generally mild side effects of sedation can include drowsiness, dizziness, nausea, or temporary memory gaps about the procedure. More serious complications are uncommon but can occur, particularly if underlying medical conditions or medication interactions are present. That is why a thorough medical review and appropriate monitoring are essential parts of any sedation plan. The dental team will explain expected side effects and when to seek immediate care.
To minimize risk, patients should fully disclose health information and follow pre- and post-procedure instructions closely. Monitoring during the visit and trained personnel ready to manage complications further reduce the likelihood of serious events. If you have specific health concerns that increase risk, the clinician will discuss alternatives or additional precautions to protect your well-being. Transparency and adherence to safety protocols are central to risk reduction.
Yes, sedation can enable longer or more complex appointments by increasing patient comfort and tolerance for extended treatment times. When a patient is relaxed, clinicians can often perform multiple procedures or more comprehensive restorations in one session, which reduces the total number of visits and the cumulative stress of repeat appointments. This can be especially useful for patients who have difficulty sitting for long periods or who experience intense anxiety with routine care. The treatment plan balances the amount of work scheduled with safety considerations and recovery needs.
Even when more work is feasible in a single visit, clinicians consider overall health, the chosen sedation level, and post-procedure recovery when planning the appointment. Some procedures still require staging for optimal healing or to reduce risk, so the dental team will recommend the safest, most effective approach. Clear pre-visit planning and coordination ensure that a longer appointment under sedation proceeds smoothly and with appropriate follow-up care.

Scheduling your next visit to Granby Dental Center is quick and hassle-free. Whether you have a specific question about our services or just need to easily book a routine cleaning, our professional staff is here to provide clear answers and simple solutions.
We’ve made it easier than ever to get in touch: give us a call or use our quick online form. Don't put your oral health on the back burner, connect with us today and let us handle the details while you focus on your smile.