Being told you need a root canal can feel alarming, but modern endodontic care is designed to end pain and preserve your natural tooth with as little discomfort as possible. Root canal therapy removes damaged or infected tissue from inside the tooth, stops the source of pain, and allows the tooth to remain in the mouth doing the job it was meant to do — biting, chewing, and preserving the jaw bone.
At Granby Dental Center, we combine up-to-date techniques with patient-focused care so that treatment is efficient and predictable. We prioritize clear explanations, gentle treatment, and follow-up care that helps patients return to normal life quickly after a procedure.
Losing a tooth can set off a cascade of changes in the mouth: neighboring teeth may drift, the bite can shift, and chewing efficiency declines. Root canal therapy is often the best way to keep a tooth functional when the inner tissues have become irreversibly injured or infected. By preserving the natural tooth, you avoid many of the long-term consequences that follow extraction.
Success rates for contemporary root canal procedures are high when treatment is performed promptly and restored appropriately afterward. The procedure eliminates the infected or inflamed pulp, cleans and seals the internal canals, and prepares the tooth for a protective restoration. This approach frequently restores comfort and function for many years.
Choosing to save a tooth through root canal therapy also supports the overall health of the mouth. Maintaining your natural tooth helps preserve the surrounding bone and keeps the forces of chewing evenly distributed across your dental arch — important for long-term oral stability and comfort.

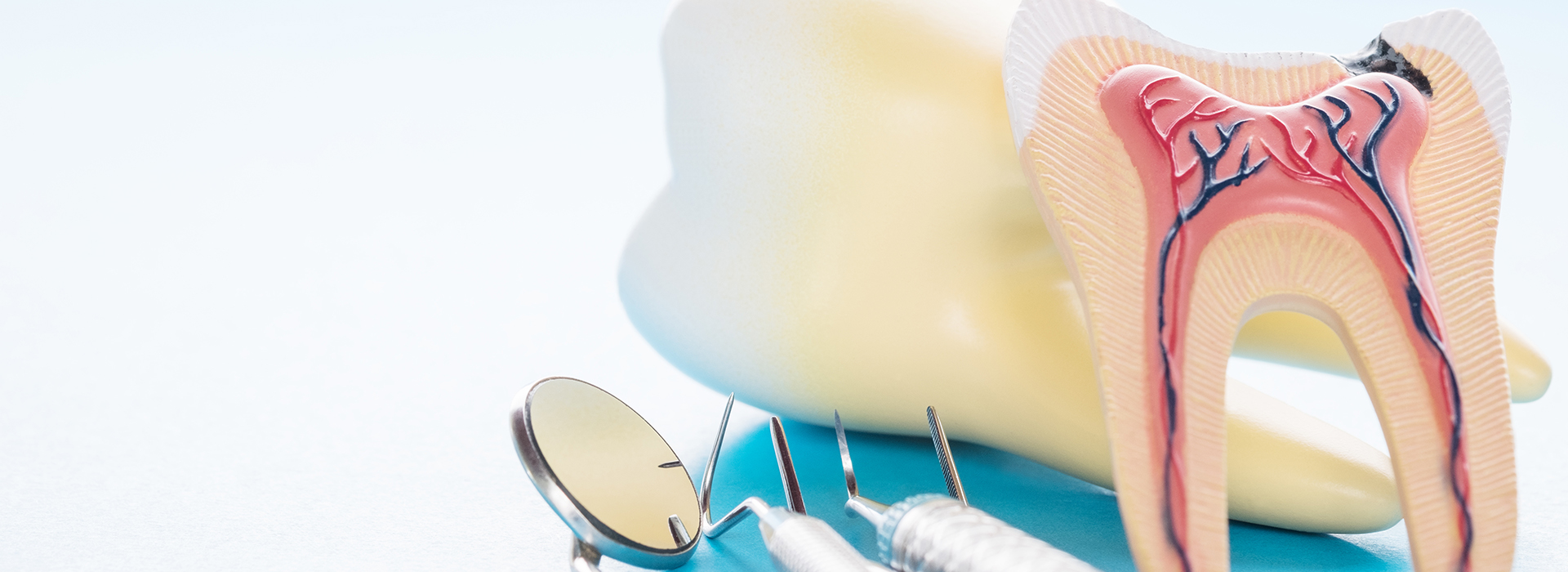
At the center of each tooth is the dental pulp: a small bundle of connective tissue, blood vessels, and nerves that help the tooth mature and sense changes in the mouth. Once a tooth is fully formed, it no longer relies on the pulp for nourishment in the same way, but the pulp remains the pathway through which infections can spread if decay or trauma reaches it.
Decay that reaches the inner chamber or a strong blow to a tooth can compromise the pulp, leading to inflammation, pain, or death of the tissue. Bacteria inside the pulp can work their way down the root canals to the surrounding bone, where an infection can produce swelling, discomfort, or a radiographic sign of root-end disease.
Because the nerve endings inside a tooth are sensitive, early involvement of the pulp often produces warning signs. Timely assessment and treatment can stop infection from spreading and often allow the tooth to be retained rather than extracted.
Not every toothache signals the need for root canal therapy, but certain patterns of symptoms suggest the inner tissues are compromised. Persistent or worsening pain, especially when it disrupts sleep or remains despite over-the-counter remedies, merits a dental evaluation. Left untreated, the source of that pain can become an infection that affects surrounding tissues.
Extreme sensitivity to hot or cold that lingers after the stimulus is removed may indicate an inflamed or dying pulp. Similarly, pain on biting or constant tenderness to pressure can reflect nerve involvement or a developing abscess. In some cases, a tooth changes color as the internal tissues break down, signaling that the tooth’s vitality has been affected.
Swelling of the gums near a tooth or drainage of pus are signs of an established infection and require timely care. If a tooth becomes mobile or the bite feels different, those are additional clues that the supporting structures may be affected and prompt treatment can improve the prognosis.
Pain that persists day after day or wakes you from sleep is a common reason patients seek care. Such pain often indicates deep decay or infection that should be evaluated without delay.
When hot or cold sensations cause sharp or prolonged discomfort, the pulp may be inflamed. Rapid diagnosis helps avoid progression to a more serious infection.
Discomfort on chewing or a tender tooth to the touch can point to canal involvement, small cracks, or localized infection that warrants assessment.
Color changes can occur when internal tissues have been damaged. A darker tooth does not always hurt, but it often reflects a loss of vitality and should be evaluated.
Injuries that expose or traumatize the inner tissues can lead to pulp damage. Even if immediate pain is mild, the affected tooth can deteriorate over time without treatment.
Localized gum swelling, tenderness, or drainage may signal an abscessed tooth. These signs should prompt a prompt dental visit to control infection and protect oral health.
If a tooth feels loose or the way your teeth come together changes, underlying infection or bone loss could be present. Treating the source can stabilize the situation.
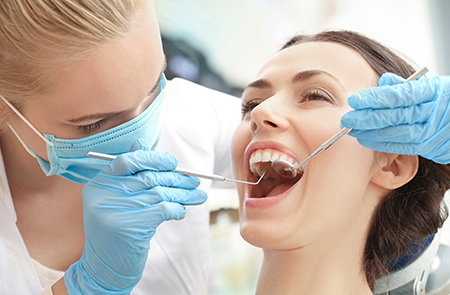
Today’s root canal procedures are performed with precise instruments and techniques that make the experience far more comfortable than in decades past. Treatment typically begins with a careful exam and imaging to understand the tooth’s anatomy and the extent of any infection. Local anesthesia reliably numbs the area so the procedure is pain-free.
The dentist accesses the pulp chamber, removes diseased tissue, cleans and shapes the canals, and then seals them with a biocompatible material. Some cases can be completed in a single visit; others require two or more appointments depending on complexity or the presence of active infection. Sedation options are available for patients who prefer extra relaxation during treatment.
After cleaning and filling the canals, the tooth will receive a temporary or permanent restoration to restore form and function. This step is crucial because a properly restored tooth resists fracture and returns to normal chewing function.
Most patients experience some tenderness in the treated area for a few days, especially once the anesthesia wears off. Over-the-counter pain relievers and following the dentist’s post-care instructions usually keep discomfort manageable. If antibiotics are prescribed, it’s important to complete the entire course as directed.
Because a tooth that has had root canal therapy can be more prone to fracture, placing a protective crown or an appropriate permanent restoration is often recommended to rebuild strength and prevent future problems. Restoring the tooth promptly supports a long-lasting result and allows you to resume full chewing function.
With timely treatment and sensible follow-up care, a tooth treated with root canal therapy can remain healthy and functional for many years — often for the remainder of a person’s life. Good oral hygiene, routine dental visits, and addressing any new symptoms early will support a favorable outcome.
Granby Dental Center is committed to providing clear information and compassionate care for patients needing endodontic treatment. If you’re experiencing symptoms or have questions about root canal therapy, please contact us for more information and to arrange an evaluation.

Root canal therapy is a dental procedure that removes damaged or infected pulp from inside a tooth, then cleans, shapes and seals the internal canals to stop infection and relieve pain. The treatment preserves the natural tooth structure so the tooth can continue to function for biting and chewing. By saving the natural tooth, root canal therapy helps maintain the surrounding bone and the proper alignment of neighboring teeth.
When performed promptly and followed by an appropriate restoration, root canal treatment often restores comfort and function for many years. At the office of Granby Dental Center, clinicians combine modern techniques with patient-focused care to make the procedure efficient and predictable.
Certain patterns of symptoms suggest the pulp inside a tooth is compromised: ongoing or severe pain that disrupts sleep, prolonged sensitivity to hot or cold, pain on biting, or noticeable darkening of a tooth. Swelling of the gums near a tooth, drainage of pus, a loose tooth or changes in your bite are also warning signs that require prompt attention. Not every ache means a root canal is necessary, but these signs merit a timely dental evaluation.
Early assessment with clinical examination and imaging helps determine whether the pulp can be saved and improves the chance of a successful outcome. If you experience persistent or worsening symptoms, contacting a dental office for an evaluation is the best course of action.
Treatment begins with a thorough exam and imaging to map the tooth’s anatomy and assess any infection. After reliable local anesthesia is administered, the dentist gains access to the pulp chamber, removes diseased tissue, cleans and shapes the root canals and seals them with a biocompatible material. The procedure may be completed in a single visit or staged across multiple appointments depending on complexity and the presence of active infection.
Modern instruments, magnification and imaging improve precision and predictability during care. Granby Dental Center offers careful treatment planning and explains each step so patients know what to expect and how the tooth will be restored afterward.
With effective local anesthesia, patients typically experience little to no pain during the procedure itself; modern techniques make the process far more comfortable than in the past. Some tenderness or mild soreness in the treated area is common for a few days after treatment as tissues settle, and this is usually manageable with over-the-counter analgesics and rest. Following post-procedure instructions helps minimize discomfort and supports healing.
If pain is severe, intensifies over time or is accompanied by swelling or fever, you should contact your dental provider promptly for reassessment. In some cases additional treatment such as antibiotics, retreatment or surgical approaches may be necessary to address persistent symptoms.
After treatment avoid chewing on the treated tooth until it has been permanently restored to reduce the risk of fracture. Maintain good oral hygiene with gentle brushing and flossing to keep the surrounding tissues healthy, and follow any specific instructions provided by your dentist regarding medications or temporary restoration care. If antibiotics are prescribed, take the full course as directed.
Schedule the recommended follow-up appointment so the tooth can receive a permanent restoration, often a crown, to rebuild strength and function. Report any persistent pain, swelling or changes in the treated tooth to your dental office right away so the situation can be evaluated.
Teeth that have undergone root canal therapy can become more brittle because some internal tissue is removed and structural tooth material may have been lost from decay or fracture. A protective crown or other appropriate permanent restoration helps reinforce the tooth, reduce the risk of fracture and restore normal chewing function. Placing a durable restoration promptly supports the long-term success of the treatment.
The choice of restoration depends on the tooth’s location, remaining tooth structure and functional demands. Your dentist will explain the recommended timing and type of restoration to balance protection, function and esthetics for the treated tooth.
When root canal treatment is performed properly and followed by a good restoration, many treated teeth remain healthy and functional for many years, often for the remainder of a person’s life. Success depends on factors such as the extent of the original infection, the quality of the restoration, the tooth’s structural integrity and ongoing oral hygiene. Regular dental checkups and prompt attention to new symptoms help detect problems early and preserve the result.
In some situations retreatment or additional procedures may be needed if symptoms recur or radiographic changes appear. Discussing expected outcomes and follow-up plans with your dentist can set realistic expectations for longevity and care.
No dental procedure is without risk, and potential complications after root canal therapy can include persistent or recurrent infection, instrument separation inside a canal, or incomplete cleaning of complex canal anatomy. In some cases a tooth may require retreatment, apical surgery or extraction if symptoms persist or new issues arise. Careful diagnosis, treatment planning and adherence to technique reduce the likelihood of complications.
If you notice ongoing pain, swelling, drainage or other concerning signs after treatment, contact your dental provider for prompt evaluation. Early intervention improves the chances of resolving complications and preserving the tooth when possible.
Extraction may be recommended when a tooth is so extensively damaged by decay, fracture or periodontal disease that it cannot be predictably restored after root canal therapy. Other reasons to consider extraction include insufficient remaining tooth structure, severe root resorption or anatomical considerations that make successful endodontic treatment unlikely. Treatment planning should weigh the benefits of saving the natural tooth against the long-term prognosis and the patient’s overall oral health.
If a tooth is extracted, replacement options such as a dental implant or bridge can restore chewing function and preserve the dental arch. Your dentist can review the comparative advantages of saving versus replacing a tooth and help you select the most appropriate treatment for your situation.
Dental practices commonly offer strategies to help anxious patients feel more comfortable during root canal treatment, including clear explanations, local anesthesia, nitrous oxide (laughing gas) and oral sedatives when appropriate. The choice of sedation depends on the patient’s medical history, anxiety level and the complexity of the procedure, and it is discussed during treatment planning. Staff will review safety considerations and any pre-appointment instructions to ensure the chosen approach is appropriate.
If you experience dental anxiety, let your provider know so they can recommend options that improve your comfort and make treatment more manageable. A collaborative approach helps tailor care to your needs while maintaining safety throughout the procedure.

Scheduling your next visit to Granby Dental Center is quick and hassle-free. Whether you have a specific question about our services or just need to easily book a routine cleaning, our professional staff is here to provide clear answers and simple solutions.
We’ve made it easier than ever to get in touch: give us a call or use our quick online form. Don't put your oral health on the back burner, connect with us today and let us handle the details while you focus on your smile.