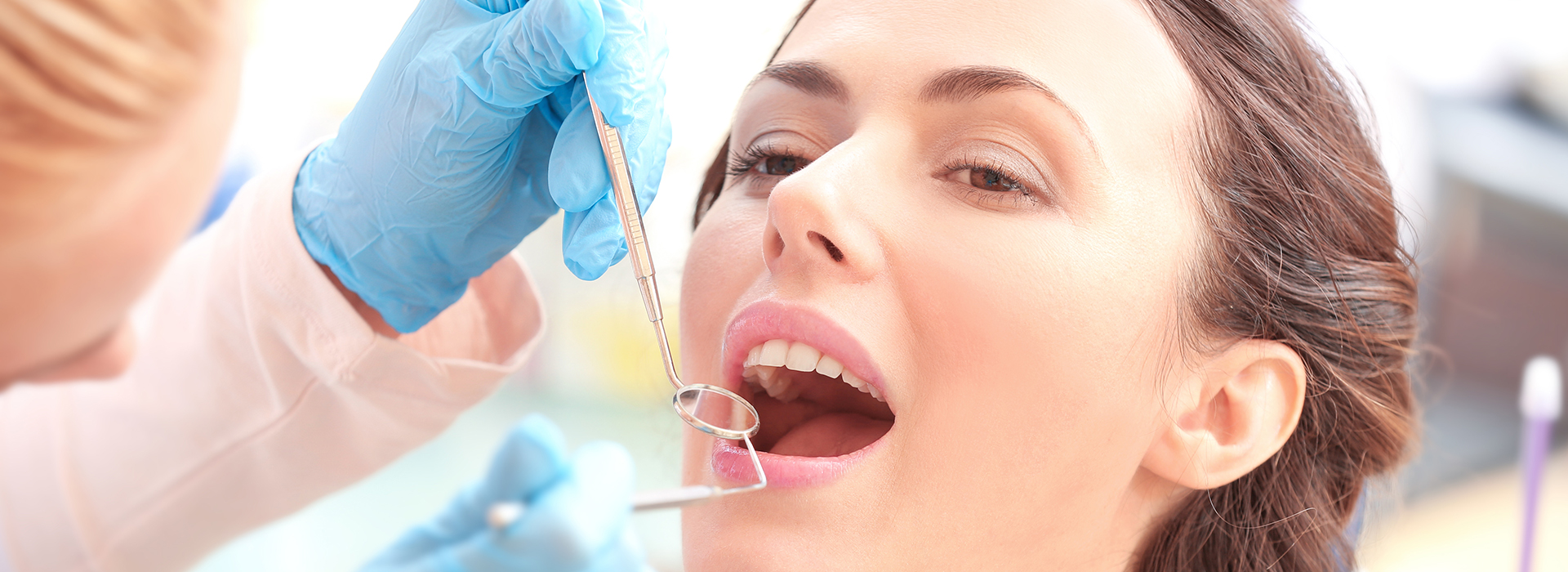
Gum disease is one of the leading reasons adults lose teeth, and many people carry early signs without realizing it. Studies from public health organizations show periodontal conditions affect a significant portion of adults nationwide. With informed care and timely attention, most cases can be controlled or reversed before they cause lasting damage. At Granby Dental Center, our approach focuses on thorough evaluation, clear explanations, and personalized treatment plans designed to protect the tissues that surround and support your teeth.
Periodontal disease starts when harmful bacteria in dental plaque irritate the gums and trigger an inflammatory response. That inflammation can progress from surface redness and swelling to deeper involvement of the fibers and bone that secure your teeth. Because the early stages are often painless, many people don’t notice a problem until more advanced changes have occurred.
Left unaddressed, chronic gum inflammation can lead to pocket formation between teeth and gums, recession of the gum line, and eventual bone loss. These changes compromise the stability of teeth and can affect chewing, speech, and the overall appearance of your smile. Beyond the mouth, emerging research links periodontal inflammation with broader health concerns, underscoring the value of maintaining periodontal health.
Recognizing the difference between simple plaque buildup and active gum disease is the first step toward protection. Regular dental exams and periodontal evaluations allow clinicians to detect early signs, measure changes over time, and recommend the least invasive treatments likely to succeed.
Gum disease does not always announce itself loudly, but there are common signals that should prompt a prompt dental evaluation. You might notice gums that redden, puff up, or bleed with routine brushing and flossing. Persistent bad breath, a metallic taste, or increased tooth sensitivity can also be related to gum irritation and bacterial activity beneath the gumline.
Physical changes such as gum recession, loose-feeling teeth, new gaps forming between teeth, or discomfort while biting are indicators that the supporting structures are being affected. Not every symptom means advanced disease, but any of these findings warrants assessment so appropriate care can be introduced before more tissue is lost.
To help patients spot problems early, we recommend paying attention to daily oral care and reporting any persistent changes to your dental provider. Professional cleanings and periodontal checks are designed to reveal hidden issues that can escape notice at home.

The earliest and most reversible form of gum disease is limited to the superficial gum tissues and is commonly called gingivitis. In this phase, the connective tissues and bone that support teeth remain intact, so with appropriate care the condition is typically reversible. Treatment focuses on controlling bacterial plaque and reducing inflammation.
Treatment for gingivitis usually involves professional cleaning to remove plaque and tartar from above and below the gumline, plus guidance on optimizing home care. Improving brushing technique, incorporating interdental cleaning, and increasing the frequency of professional maintenance can halt disease progression and restore healthy gum tissues.
Because gingivitis is often symptom-light, routine dental visits are essential. When identified early, relatively simple interventions can prevent the transition to more destructive stages that require more involved therapies.

When inflammation persists and moves deeper, the condition progresses to periodontitis. At this stage, the bacterial assault and body’s inflammatory response begin to break down the fibers and bone that hold teeth in place. The result can be deeper periodontal pockets, shifting teeth, and long-term loss of support.
Management of periodontitis aims to stop active disease, reduce pocket depths, and restore as much healthy architecture as possible. Depending on the severity, care may include targeted antimicrobial therapy, mechanical cleaning below the gumline, and procedures to encourage tissue regeneration.
Prompt, staged treatment combined with a strong maintenance routine helps minimize further tissue loss and preserves function. With current techniques, many people regain stable periodontal health and avoid the need for tooth removal.
Contemporary periodontal treatment emphasizes tailored care that matches the individual patient’s needs. After a full assessment, your dental team will recommend the least invasive yet most effective options—ranging from enhanced professional cleaning and localized antimicrobial application to surgical approaches for persistent disease.
When deeper treatment is required, clinicians can employ procedures that clean infected root surfaces, reduce pocket depth, and, where appropriate, use grafting or regenerative materials to encourage bone and tissue repair. Advances such as laser-assisted therapy may be included for specific indications, always within the context of an evidence-based plan.
Success depends not only on the procedure but also on consistent follow-up and a disciplined home-care program. Long-term maintenance visits are scheduled to monitor healing, remove recurring deposits, and reinforce techniques that keep disease at bay.
When periodontal disease is detected before extensive tissue loss, conservative measures are the first line of action. These treatments aim to eliminate harmful biofilm and tartar from beneath the gumline while preserving healthy tissue. Effective non-surgical care can stop progression and improve pocket depths without incisions or sutures.
Scaling and root planing—deep cleaning of root surfaces—removes the source of irritation and allows inflamed gums to heal and reattach more securely. In selected cases, topical or systemic antimicrobials are used as adjuncts to reduce bacterial load and support healing.
Non-surgical pathways prioritize outcomes that are predictable and carry less recovery time, but they require patient commitment to meticulous home care and periodic professional maintenance to remain effective.
When pockets deepen beyond what can be cleaned effectively with non-surgical methods, or when structural repair is needed, periodontal surgery may be recommended. Surgical procedures provide direct access to the roots and bone, allowing thorough debridement and reshaping of the supporting tissues.
Common surgical goals include removing persistent deposits, reducing pocket depth, recontouring damaged bone, and, when appropriate, placing grafts to rebuild lost tissues. Flap procedures are widely used to expose roots for cleaning and to position tissues for optimal healing.
With modern techniques and careful post-operative care, surgical interventions can significantly improve the mouth’s ability to stay cleanable and healthy, lowering the long-term risk of tooth loss and related complications.
Maintaining periodontal health is a partnership between your care team and you. At Granby Dental Center, we focus on listening to your concerns, explaining options clearly, and creating a plan that preserves your smile’s function and appearance. If you’d like more information about periodontal care or want to discuss an individualized plan, please contact us for more information.

Periodontal disease is an infection and inflammation of the gums and the supporting structures that surround the teeth. It begins when bacterial plaque accumulates along the gumline and triggers an immune response that damages soft tissues. Over time, untreated inflammation can extend to the fibers and bone that anchor teeth, reducing stability.
Early stages may be limited to reversible gum inflammation, while progressive stages lead to pocketing, recession, and bone loss. Because early disease is often painless, routine exams are essential for detection before irreversible changes occur. Effective care focuses on removing bacterial deposits and managing inflammation to protect oral health.
Common early warning signs include gums that bleed during brushing or flossing, persistent bad breath, and gums that appear red or swollen. Some patients also notice increased tooth sensitivity or a metallic taste, which can indicate bacterial activity beneath the gumline. These symptoms should prompt a periodontal evaluation even when pain is absent.
Physical changes such as gum recession, loose-feeling teeth, or new gaps between teeth can signal advancing disease and warrant prompt attention. A clinician will assess pocket depths and attachment levels to determine the severity and plan appropriate care. Early recognition and treatment improve the chances of restoring healthy tissues.
Diagnosis starts with a comprehensive clinical exam that measures pocket depths, evaluates attachment loss, and inspects soft tissues for inflammation. Dental X-rays help reveal bone levels and patterns of loss that are not visible during an exam, while medical and dental history informs risk factors such as smoking or diabetes. Together these findings allow clinicians to stage disease and tailor treatment recommendations.
Periodontal charting and regular comparisons over time are important to monitor progression and treatment response. Your dental team may use adjunctive tests such as microbial sampling or inflammation markers in select cases to refine therapy. Accurate diagnosis guides whether conservative care or more advanced intervention is needed.
Non-surgical periodontal therapy is the first line of treatment for many patients and centers on thorough removal of plaque and calculus from root surfaces. Scaling and root planing under local anesthesia reduces bacterial load and allows inflamed tissues to heal and reattach more firmly. In-office procedures are complemented by improved home care, including targeted brushing and interdental cleaning.
Adjunctive measures such as localized antimicrobial delivery or short courses of systemic medication may be used selectively to reduce specific pathogens. Regular periodontal maintenance visits help sustain treatment gains by removing recurring deposits and monitoring tissue stability. Consistent patient commitment to hygiene and recall appointments is essential for long-term success.
Surgical periodontal therapy is considered when non-surgical approaches cannot adequately control deep pockets or when structural repair is necessary. Common procedures include flap surgery to expose and clean root surfaces, osseous recontouring to reshape damaged bone, and grafting to restore lost tissue volume. These interventions provide better access for debridement and create conditions that favor regeneration and easier home care.
Regenerative techniques may employ bone grafts, barrier membranes, or biologic agents to encourage new attachment where appropriate. Careful case selection and post-operative management are critical to optimize healing and preserve function. When indicated, surgery can greatly improve long-term prognosis and reduce the risk of tooth loss.
Antibiotics and adjunctive therapies are tools that support mechanical cleaning rather than replace it; they are chosen based on disease severity and individual patient needs. Localized antimicrobials can be placed directly into periodontal pockets to concentrate the effect, while systemic medications are reserved for more widespread or aggressive infections. Host-modulation therapies, which aim to reduce destructive inflammation, are an option in selected situations.
Laser-assisted treatments may be used as adjuncts to reduce microbial burden and promote healing when clinically appropriate. Any adjunctive therapy should be evidence-based and integrated into an overall treatment plan that includes mechanical debridement and maintenance. Your clinician will explain the rationale, expected benefits, and limitations of additional therapies so you can make an informed decision.
Periodontal inflammation can have effects beyond the mouth, and mounting research links gum disease with systemic conditions such as diabetes and cardiovascular disease. While causal relationships are complex and still under study, controlling oral inflammation is an important part of overall health maintenance for patients with chronic medical conditions. Effective periodontal care may improve glycemic control in people with diabetes and reduce inflammatory burden systemically.
The team at Granby Dental Center coordinates with medical providers when systemic factors influence periodontal risk or treatment response. Managing modifiable risk factors—such as tobacco use and uncontrolled blood sugar—enhances the effectiveness of periodontal therapy. Patients with complex medical histories benefit from an individualized approach that balances dental treatment with general health considerations.
Recovery after periodontal treatment depends on the procedures performed but typically includes short-term discomfort, mild swelling, and changes in eating habits that resolve with time. Pain is usually managed with over-the-counter analgesics and recommended oral hygiene modifications, and clinicians provide specific post-operative instructions to support healing. Adhering to follow-up visits allows the team to monitor progress and intervene early if healing deviates from the expected course.
For surgical cases, patients may receive temporary dietary and activity recommendations and guidance on gentle cleaning techniques to protect healing sites. Sutures are removed or monitored according to the clinician’s timeline, and gradual improvement in pocket depths and tissue health is expected over several weeks to months. Long-term stability relies on disciplined home care and regular professional maintenance.
Preventing recurrence of periodontal disease requires a partnership between patients and their dental team focused on daily plaque control and risk management. Effective strategies include twice-daily brushing with a technique that reaches the gumline, daily interdental cleaning with floss or interdental brushes, and quitting tobacco use. Addressing systemic factors like diabetes control and reducing stress can also lower the risk of relapse.
Periodic periodontal maintenance appointments allow clinicians to remove new deposits, reassess periodontal status, and reinforce home-care techniques. The frequency of maintenance is individualized based on risk and treatment response but is often more frequent than routine dental cleanings. Staying engaged with the care plan is the most reliable way to preserve treatment results and maintain oral health.
At Granby Dental Center, we begin personalized planning with a full assessment that includes clinical measurements, radiographs, and a review of medical history and risk factors. This comprehensive baseline enables the team to stage disease accurately and select the least invasive options likely to succeed. Treatment pathways are discussed with patients so goals, expectations, and responsibilities are clear from the outset.
Plans are adjusted based on treatment response, patient preferences, and changes in health status, with ongoing monitoring to detect recurrence early. Emphasis is placed on patient education, tailored maintenance intervals, and coordination with other healthcare providers when systemic issues affect periodontal health. This collaborative, evidence-based approach helps patients achieve stable, long-term results.

Scheduling your next visit to Granby Dental Center is quick and hassle-free. Whether you have a specific question about our services or just need to easily book a routine cleaning, our professional staff is here to provide clear answers and simple solutions.
We’ve made it easier than ever to get in touch: give us a call or use our quick online form. Don't put your oral health on the back burner, connect with us today and let us handle the details while you focus on your smile.