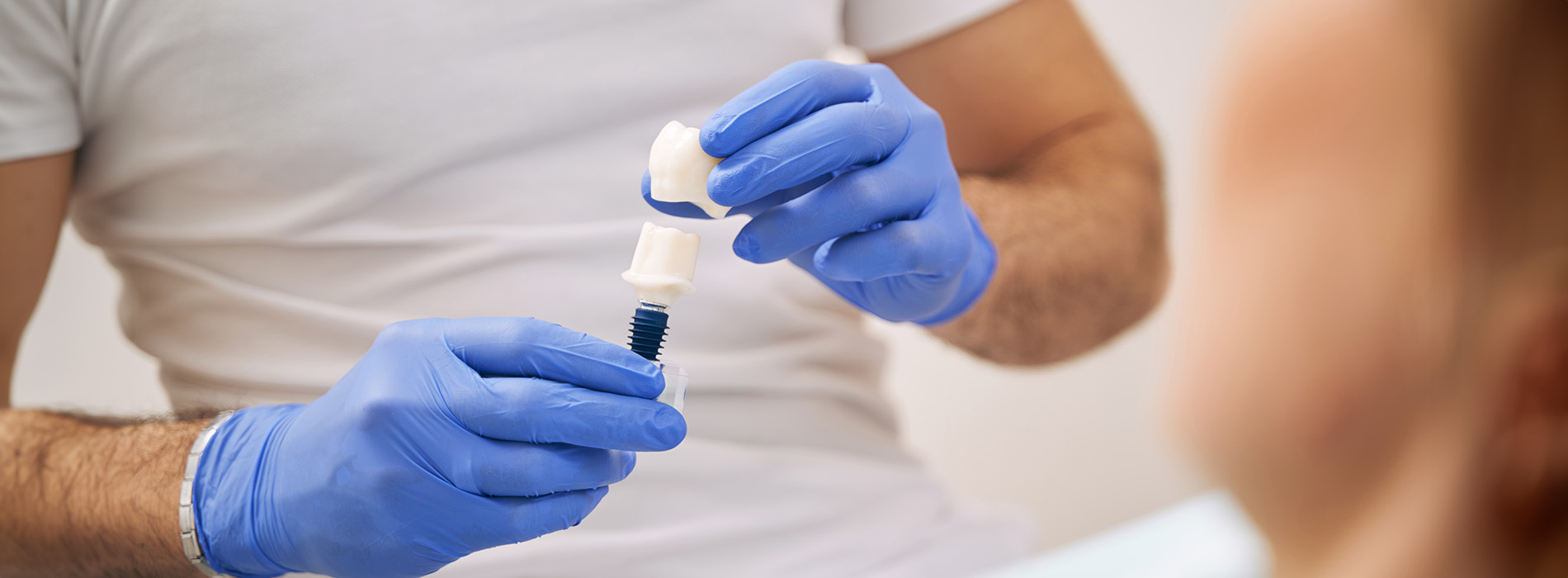
An implant-supported crown replaces a single missing tooth with a solution that looks, feels, and functions like the original. Unlike restorations that rely on neighboring teeth for support, an implant-supported crown is anchored by a small titanium post that fuses with the jawbone, creating a stable foundation for a custom-crafted crown. This approach restores chewing function, preserves facial structure, and offers a long-term alternative to traditional bridges and removable appliances.
An implant-supported crown is the visible portion of a three-part system: the implant (the titanium post), the abutment (a connector), and the crown (the prosthetic tooth). The implant is surgically placed in the jaw where the natural tooth root once was. Over time the surface of the implant bonds with the surrounding bone in a process called osseointegration, creating a durable attachment that behaves much like a natural root.
The abutment joins the implant to the crown and is selected to match the specific clinical situation — angled or straight, prefabricated or custom-made. The crown itself is shaped and shaded to match the patient’s neighboring teeth, restoring a natural appearance while reestablishing normal bite contacts. Because each element is designed to work in concert, the result is both functional and esthetic.
Because the implant occupies the site of the missing root, it helps maintain the surrounding bone and gum contours. That foundation supports both the crown’s stability and the long-term health of the jaw. For patients seeking a replacement that minimizes the involvement of adjacent teeth, an implant-supported crown is often the most conservative restorative option.
One of the key benefits of an implant-supported crown is that it leaves neighboring teeth untouched. Traditional fixed bridges require at least two adjacent teeth to be prepared and fitted with crowns to support a false tooth between them. That process removes healthy tooth structure and can increase the risk of future problems for those supporting teeth. By contrast, an implant stands independently, preserving the integrity of surrounding teeth.
Beyond protecting adjacent teeth, dental implants help prevent the progressive bone loss that follows tooth extraction. When a natural root is gone, the jawbone begins to resorb without the mechanical stimulation provided by chewing. An implant transmits forces to the bone in a way similar to a natural tooth root, helping to preserve bone volume and maintain facial proportions over time.
Maintaining proper bite alignment is another long-term advantage. A single missing tooth left unaddressed can allow neighboring teeth to drift and opposing teeth to over-erupt, which can lead to occlusal changes and increased wear. An implant-supported crown restores the vertical dimension and helps keep the bite balanced, reducing the likelihood of secondary restorative needs down the road.
The journey to an implant-supported crown begins with a thorough evaluation. Digital X-rays and, when indicated, three-dimensional imaging help the dental team assess bone quality, nerve locations, and sinus anatomy. A careful review of medical and dental history ensures the chosen plan accounts for overall health, habits such as smoking, and any medications that could affect healing.
Surgical placement of the implant is typically performed with attention to comfort and precision. Depending on the case, this can be a one-visit procedure under local anesthesia or combined with sedation for added relaxation. After the implant is seated in the jaw, a period of healing follows during which the bone integrates with the implant surface. This phase usually lasts several weeks to a few months and is essential for long-term stability.
Once osseointegration is complete, the abutment is attached and precise impressions are taken to craft the final crown. Modern workflows may use digital scans to design a restoration that matches neighboring teeth in shape, size, and color. The crown is then secured to the abutment and adjusted for a comfortable bite, finalizing a restoration that provides both function and esthetics.
Throughout treatment the dental team monitors healing and guides aftercare. While timelines vary by individual, clear communication and careful planning ensure predictable outcomes and help patients understand what to expect at each stage.
Crowns for implant restorations are made from materials chosen to balance durability and natural appearance. Porcelain-fused-to-zirconia, full-contour zirconia, and lithium disilicate are common choices, each offering a combination of strength and lifelike translucency. The selection depends on the location of the tooth, bite forces, and aesthetic goals — for example, an anterior crown may prioritize translucency while a molar crown emphasizes strength.
Color matching and contouring are integral to creating a seamless result. Shade selection considers not only the visible tooth color but also underlying tooth structure, gum tone, and even the patient’s smile dynamics. Skilled laboratory work and careful on-site adjustments ensure the crown blends with adjacent teeth and looks natural at rest and in motion.
Longevity depends on both material choice and ongoing care. With proper hygiene, routine dental visits, and attention to protective measures like nightguards when indicated, implant-supported crowns can last many years. The underlying implant is designed to be a permanent solution, while the crown may require replacement at some point due to wear or cosmetic changes — a predictable aspect of long-term restorative dentistry.
Caring for an implant-supported crown is similar to caring for natural teeth. Daily brushing with a soft-bristled brush and interdental cleaning with floss or interdental brushes helps prevent plaque buildup around the crown and abutment. Using non-abrasive toothpaste and avoiding overly aggressive scrubbing protects both the restoration and surrounding soft tissues.
Regular dental checkups and professional cleanings are essential to monitor the health of the implant and the integrity of the crown. During these visits, the dentist will assess gum health, check for signs of wear or looseness, and evaluate the opposing teeth to ensure the bite remains balanced. Early detection of potential issues allows simple interventions before problems escalate.
Occasional sensitivity, minor staining, or normal wear can be managed with routine care, but certain signs warrant prompt attention. Persistent discomfort, unusual mobility of the crown, or swelling in the gums around the implant should be evaluated as soon as possible. Timely professional assessment helps protect both the restoration and the underlying implant, preserving the investment in oral health.
In summary, an implant-supported crown is a durable, conservative way to replace a single missing tooth while protecting adjacent teeth and preserving jawbone health. The process involves careful planning, precise surgical placement, and a custom-fitted crown designed for long-term function and appearance. If you’d like to learn how this treatment might apply to your smile, please contact Granby Dental Center for more information.

An implant-supported crown replaces a single missing tooth with a prosthetic that mimics the form and function of a natural tooth. The restoration is secured to a titanium implant that is surgically placed in the jaw and allowed to integrate with bone. Because the replacement includes a root-like foundation, it restores chewing function and maintains the surrounding gum contours.
This approach differs from restorations that rely on adjacent teeth for support, so neighboring teeth are not altered to hold the replacement. The visible crown is custom shaped and shaded to blend with adjacent teeth, providing a natural appearance. When planned and placed correctly, an implant-supported crown offers a stable, conservative long-term solution for replacing one tooth.
The implant, abutment and crown form a three-part system that recreates the structure of a natural tooth. The titanium implant acts as a root and becomes integrated with the jawbone through osseointegration, creating a stable foundation. The abutment is a connector that fastens to the implant and supports the prosthetic crown.
The crown is designed to match the size, shape and color of neighboring teeth and is attached to the abutment for proper bite contact. Each component is selected to suit the clinical situation, with options for angled or custom abutments when needed. Together the elements restore function, esthetics and long-term support for the surrounding tissues.
An implant-supported crown preserves the integrity of adjacent teeth because it does not require preparing healthy tooth structure to support a replacement. Fixed bridges typically depend on crowns placed on neighboring teeth, which can increase the risk of future restorative work on those teeth. An independent implant avoids that trade-off and maintains more of your natural dentition.
Implants also help preserve the underlying jawbone by transmitting chewing forces that stimulate bone health. That preservation of bone volume helps maintain facial proportions and reduces the risk of shifts in tooth position over time. For many patients seeking a single-tooth replacement, an implant-supported crown offers a more conservative and biologically favorable option.
Candidacy for an implant-supported crown depends on several factors including overall health, bone volume at the treatment site and oral habits. Adequate bone is needed to support the implant, and medical conditions that affect healing may influence the treatment plan. A history of heavy smoking or poorly controlled systemic conditions can increase the risk of complications and should be discussed with the dental team.
A thorough evaluation with digital imaging and a review of medical and dental history determines whether an implant is the best option or if preparatory procedures such as bone grafting are required. Many patients who initially lack sufficient bone may become candidates after site augmentation. The treatment plan is individualized to balance long-term success and the patient’s overall health.
The process typically begins with a comprehensive consultation that includes digital X-rays or 3-D imaging to evaluate bone, nerve positions and neighboring anatomy. Planning includes selecting the implant size and type and determining whether any preparatory procedures are needed. Surgical placement of the implant is performed under local anesthesia and may include sedation options for added comfort.
After placement there is a healing phase while the implant integrates with bone, which can take several weeks to a few months depending on the site and the individual. Once integration is confirmed, the abutment is attached and impressions or digital scans are taken to fabricate the final crown. Final seating of the crown is followed by bite adjustments and periodic follow-up to monitor healing and function.
Dentists commonly use full-contour zirconia, porcelain-fused-to-zirconia and lithium disilicate for implant crowns, each offering a different balance of strength and esthetics. Full-contour zirconia provides high strength for posterior teeth where chewing forces are greatest. Lithium disilicate and layered ceramic options offer greater translucency and lifelike appearance for visible front teeth.
Material selection also depends on occlusion, opposing restorations and the thickness needed to achieve both durability and a natural look. Shade matching and contouring are critical to blend the crown with adjacent teeth and gums. A skilled laboratory workflow combined with intraoral adjustments helps ensure a seamless and long-lasting result.
Implant-supported crowns are designed for longevity, and with proper care they can last many years while the implant itself is intended as a long-term solution. The crown material and the patient’s oral habits influence how long a specific restoration will remain serviceable. Over time, crowns may need replacement due to wear, fracture or changes in esthetics, which is a normal part of restorative care.
Factors that affect lifespan include oral hygiene, regular professional maintenance, bite forces and parafunctional habits such as clenching or grinding. Protective measures such as nightguards and timely management of opposing tooth wear help extend service life. Regular dental visits allow early detection of wear or changes so repairs or replacements can be planned proactively.
Home care for an implant-supported crown mirrors care for natural teeth and focuses on preventing plaque accumulation around the abutment and gumline. Daily brushing with a soft-bristled brush and the use of floss or interdental brushes help clean the area where the crown meets the gum. Using non-abrasive toothpaste and gentle technique protects both the restoration and surrounding soft tissues.
Avoiding excessively hard foods and minimizing habits that stress the restoration reduces risk of fracture or loosening. Tobacco use can compromise gum health around implants and should be discussed with your dental team. Regular professional cleanings and periodic examinations are essential to monitor tissue health and the integrity of the restoration.
While implant treatment is predictable, patients should be alert for signs that may indicate a complication, such as persistent pain, swelling, drainage or increasing redness around the implant. Mobility of the crown or implant, new or worsening bite changes and difficulty chewing also warrant immediate evaluation. Early recognition helps the dental team address issues before they compromise the implant.
Peri-implant mucositis and peri-implantitis are inflammatory conditions that affect tissue and bone around implants and require professional assessment and treatment. Routine monitoring, good plaque control and prompt attention to symptoms reduce the likelihood of progressive problems. If concerns arise, contacting the treating dentist quickly allows for timely interventions that protect both the implant and surrounding structures.
To begin, schedule a consultation so the dental team can review your medical and dental history, perform a clinical exam and obtain necessary imaging such as digital X-rays or 3-D scans. This evaluation establishes whether an implant is appropriate and identifies any site preparation needs like bone grafting. The clinician will then explain the recommended sequence of care and the expected timeline for each phase.
Bring a list of current medications and any recent dental records to the appointment to help the team plan safely and efficiently. After the initial consultation, the practice provides a personalized treatment plan and schedules the surgical and restorative appointments needed to complete the crown. Ongoing follow-up visits ensure the implant and restoration remain healthy and functional over time.

Scheduling your next visit to Granby Dental Center is quick and hassle-free. Whether you have a specific question about our services or just need to easily book a routine cleaning, our professional staff is here to provide clear answers and simple solutions.
We’ve made it easier than ever to get in touch: give us a call or use our quick online form. Don't put your oral health on the back burner, connect with us today and let us handle the details while you focus on your smile.