Missing teeth change more than your smile — they affect how you eat, speak, and how your face is supported. Modern dental implants are designed to replace both the visible tooth and its root, restoring stability and function in a way that traditional prosthetics often cannot. Because implants integrate with the jawbone, they recreate the foundation that natural teeth rely on for normal chewing forces and facial support.
Implants are made from biocompatible materials that bond with bone over time, producing a durable connection that can support a single crown, a bridge, or a full arch of replacement teeth. This biologic fusion is a key reason implants perform and feel closer to natural teeth than removable alternatives. For many patients, that translates to fewer limitations when eating and more confidence when speaking or smiling.
Clinical outcomes and patient satisfaction have driven implant dentistry to become a standard option for tooth replacement. The process is evidence-based and adaptable: dentists can tailor treatment to each person’s anatomy, health history, and aesthetic goals. At Granby Dental Center, we focus on restoring both function and appearance so patients can get back to everyday life with greater ease.

A dental implant begins as a small, precision-engineered post placed into the jawbone. Over the following weeks to months, the surrounding bone remodels and attaches itself to the implant surface in a process called osseointegration. This fused interface becomes a stable anchor capable of supporting restorative components such as crowns, bridges, and dentures.
Implant restorations are modular: the surgically placed post, an abutment that connects the post to the prosthesis, and the visible crown or denture all combine to recreate tooth form and function. Because the implant replaces the missing root, it restores the mechanical load to the bone, which helps maintain bone volume and facial structure over time — a meaningful advantage compared with solutions that only replace the visible tooth.
Precision planning is central to predictable outcomes. Contemporary implant therapy relies on diagnostic imaging and careful treatment planning to determine implant size, angulation, and position. That planning guides a surgical approach that emphasizes safety, comfort, and long-term success.
One of the most immediate benefits patients report after implant treatment is improved chewing ability. Because an implant is fixed in the jaw, it transmits bite forces in a way that feels natural and secure, making it easier to enjoy a broader variety of foods without worrying about prosthesis movement.
Implants also support clearer speech and a more comfortable fit compared with many removable appliances. For individuals who have struggled with denture slippage or recurrent adhesive use, implant-supported restorations offer a significant improvement in daily life and self-assurance.
Beyond comfort and function, implants help preserve the health of surrounding tissues. They maintain stimulation in the jawbone where teeth are missing, which reduces the progressive bone loss that can occur after extractions. Maintaining bone volume preserves facial contours and supports long-term oral health.
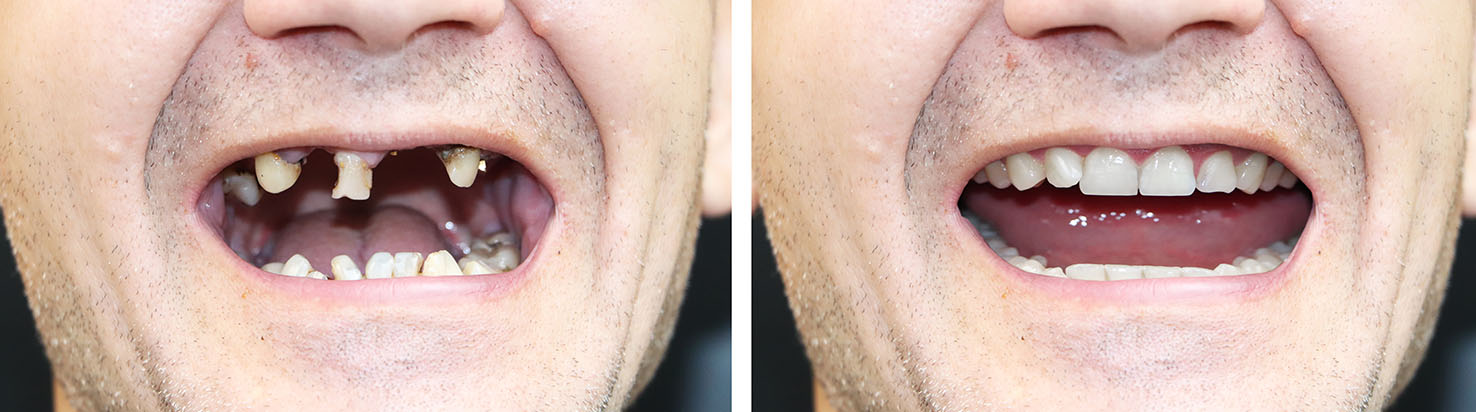
Implant dentistry is versatile: it can address a single missing tooth, several missing teeth, or a complete arch. The choice of restoration reflects how many teeth are absent, the condition of the surrounding bone, and a patient’s preferences for fixed or removable solutions. Dentists design each plan to balance longevity, esthetics, and function.
Good candidates for implant treatment have sufficient bone to support an implant and are in acceptable overall health. Factors such as chronic medical conditions, smoking, and uncontrolled periodontal disease can influence candidacy, but many patients still qualify after preparation or adjunctive therapies. A thorough evaluation helps identify the best pathway for each individual.
Implant placement is typically performed in a dental office under local anesthesia, and many patients report minimal discomfort. The exact treatment timeline varies: some cases allow for same-day provisional restorations, while others require a healing period to ensure stable osseointegration before final crowns or bridges are attached. Throughout treatment, clear communication about anesthesia options, recovery expectations, and aftercare is essential.
Bone grafting is sometimes recommended when natural bone volume is insufficient to support an implant. Grafting rebuilds the site so an implant can be placed predictably and long-term stability is achieved. These procedures are common and routinely performed when indicated to create the foundation required for success.
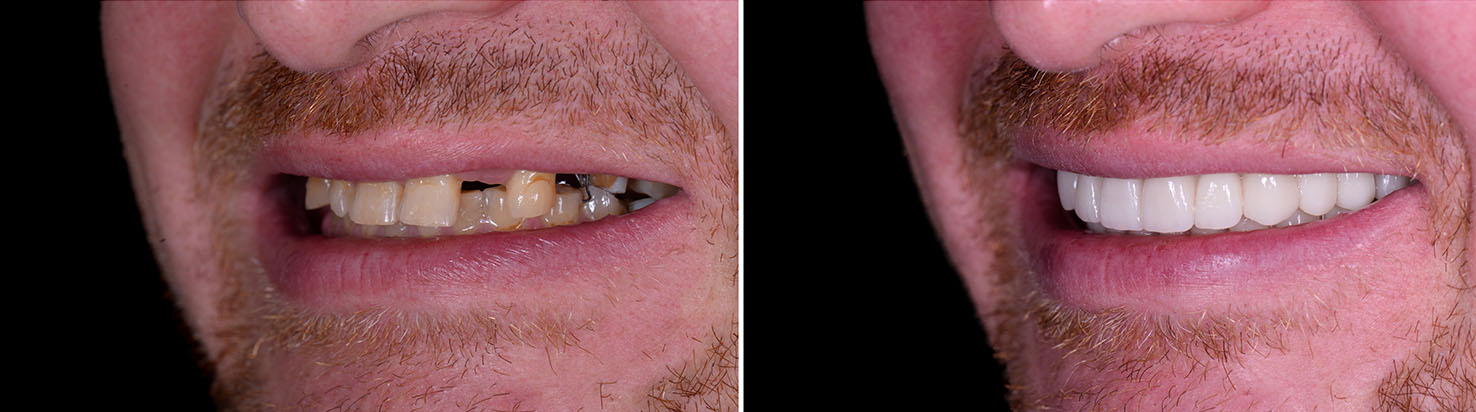
Once implants and their restorations are in place, routine home care and regular dental visits are important for long-term success. Professional exams and cleanings help detect issues early and ensure that both the implant and surrounding tissues remain healthy. With careful maintenance, implants can last for many years and become a stable, functional part of daily life.
Our team emphasizes detailed treatment planning and clear patient education so everyone understands each step of the process. That focus on communication and quality workmanship supports predictable outcomes and helps patients make informed decisions about their oral health.
Rebuilding a smile with dental implants restores more than appearance — it restores the ability to eat, speak, and interact with confidence. If you’d like to explore whether implants are the right choice for your situation, our team at Granby Dental Center can help evaluate your needs and outline a personalized treatment plan.
Contact us to learn more about implant dentistry and how modern tooth replacement can improve the comfort, function, and appearance of your smile. We’re happy to answer your questions and guide you through the next steps.

A dental implant is a biocompatible post placed into the jaw to replace a missing tooth root and provide a stable foundation for a visible restoration. The implant integrates with the surrounding bone through a process called osseointegration, creating a strong connection that supports normal chewing forces. Because the implant replicates the role of a natural root, the attached crown, bridge, or denture can function and feel like a natural tooth.
Implant restorations are modular and typically include the implant post, an abutment that connects the post to the prosthesis, and the crown or denture that restores appearance and function. The surgical post is placed into the bone, the abutment joins the post to the prosthetic component, and the visible restoration is designed to match neighboring teeth. Modern imaging and planning tools help clinicians position implants precisely for predictable, long-term outcomes.
Patients commonly experience improved chewing efficiency and clearer speech because implants are fixed and transfer bite forces in a natural way. This stability reduces concerns about slippage or movement that can occur with removable appliances and allows people to enjoy a wider variety of foods. The enhanced comfort and function often translate to greater confidence when eating and speaking.
Implants also help preserve jawbone health by restoring the mechanical stimulation that natural roots provide, which can slow or prevent the bone loss that follows tooth loss. They often spare adjacent healthy teeth from being altered for support, a common downside of traditional bridgework. With consistent home care and professional maintenance, implants offer durable performance and predictable function over time.
Good candidates generally have adequate jawbone volume, healthy gum tissue, and overall health that supports oral surgery and healing. Certain medical conditions, uncontrolled periodontal disease, and tobacco use can affect candidacy, but many patients can qualify after preparatory treatments or health management. A thorough clinical exam and diagnostic imaging are essential to determine individual suitability.
Age alone is rarely a limiting factor; biological health and bone quality are the primary considerations. When bone volume is insufficient, grafting procedures can often rebuild the site so implant placement becomes possible. Your dentist will review health history, imaging results, and treatment options to create a safe, personalized plan.
Treatment starts with a consultation that includes a clinical exam, medical history review, and diagnostic imaging to plan implant position, size, and angulation. Based on that plan, the clinician will explain the surgical steps, timeline, and which restorative option best matches your functional and aesthetic goals. In many cases a temporary restoration can be offered while the implant integrates, but final prosthetics are attached once stability is confirmed.
Surgery is commonly performed with local anesthesia and may include sedation options for added comfort; most patients report only mild discomfort during recovery. The implant post is placed into the bone and the site is allowed to heal while osseointegration occurs, with follow-up visits to monitor progress. Granby Dental Center emphasizes clear communication about anesthesia, recovery expectations, and aftercare to support predictable results.
Initial soft tissue healing usually takes a few days to a week, during which mild swelling and soreness are normal and manageable with recommended care. The biologic integration of the implant with bone (osseointegration) commonly requires several weeks to a few months depending on the site and individual healing capacity. Follow-up visits allow the clinician to track healing and determine when a final restoration can be placed.
Some treatment plans permit immediate provisional teeth that restore appearance and basic function while the implant heals, but patients may need to adjust eating habits temporarily to protect the surgical site. Final crowns or bridges are attached once the clinician confirms sufficient stability. Adhering to post-operative instructions and maintaining good oral hygiene are important for a smooth recovery and long-term success.
Bone grafting is recommended when there is insufficient jawbone volume or unfavorable ridge contours that would compromise implant placement or aesthetic results. The graft material may come from the patient’s own bone, from donor sources, or from synthetic substitutes depending on the clinical situation. Grafting rebuilds volume and shape so an implant can be positioned predictably and securely.
Common grafting procedures include socket preservation, ridge augmentation, and sinus lifts for the upper posterior jaw where height is limited. These procedures are planned with diagnostic imaging to choose the most appropriate technique for the anatomy involved. After grafting, the site is allowed to heal and integrate before implant placement, which often improves long-term implant prognosis.
Implant restorations range from single-tooth crowns to implant-supported bridges, implant-retained removable dentures, and full-arch fixed prostheses supported by multiple implants. Single implants replace an individual tooth without altering adjacent teeth, while implant-supported bridges replace several teeth using implants as independent supports. Full-arch solutions can restore an entire dental arch with a permanently attached prosthesis when appropriate.
Removable options that clip onto implant attachments provide improved retention and easier hygiene for some patients, while fixed solutions offer a permanently attached restoration that closely mimics natural teeth. The choice between fixed and removable depends on bone support, patient preference, hygiene ability, and functional goals. Your dentist will review each option’s advantages and help you select the restoration that best fits your needs.
Implants often preserve adjacent healthy teeth because they replace missing roots and provide independent support rather than relying on neighboring teeth for retention. This helps maintain bone volume and reduces the likelihood of progressive bone loss at the site of the missing tooth or teeth. While bridges and dentures remain viable treatments, implants are frequently preferred when long-term bone preservation and independent support are priorities.
Compared with conventional removable dentures, implant-supported solutions deliver greater stability, improved chewing efficiency, and fewer concerns about slippage during everyday activities. Removable dentures may still be appropriate for some patients due to anatomic or personal factors, and implant-retained dentures combine many benefits of both approaches. A careful clinical assessment helps determine which solution best balances function, aesthetics, and maintenance for each patient.
As with any surgical procedure, implant therapy carries risks such as infection, delayed healing, and inflammation around the implant if oral hygiene or systemic health is suboptimal. Nerve or sinus complications are uncommon but can occur when implants are placed near critical anatomical structures, which is why thorough planning and imaging are essential. Prompt identification and management of early signs of trouble tend to improve outcomes.
Long-term complications may include peri-implant mucositis and peri-implantitis, inflammatory conditions related to plaque accumulation around the implant. These conditions are often preventable with diligent home care and routine professional maintenance, and they may require targeted periodontal treatment if they develop. Your dental team will explain risk reduction strategies and monitoring protocols to protect implant health.
Caring for implants relies on thorough daily brushing, interdental cleaning, and regular professional examinations much like the care recommended for natural teeth. Specialized brushes, floss threaders, or water irrigation devices may be advised to clean around abutments and under fixed prostheses. Routine visits allow the clinician to assess soft tissue health, check occlusion, and perform professional cleaning to remove hardened deposits.
Avoiding tobacco, managing chronic medical conditions, and following the individualized maintenance schedule provided by your dentist all support long-term implant success. The team at Granby Dental Center can provide tailored oral hygiene instructions and recall plans to help preserve implant health and function. Consistent care and early attention to any changes are the best defenses against implant-related problems.

Scheduling your next visit to Granby Dental Center is quick and hassle-free. Whether you have a specific question about our services or just need to easily book a routine cleaning, our professional staff is here to provide clear answers and simple solutions.
We’ve made it easier than ever to get in touch: give us a call or use our quick online form. Don't put your oral health on the back burner, connect with us today and let us handle the details while you focus on your smile.