
Having a tooth taken out can feel daunting, but it’s often a straightforward path toward protecting your long-term oral health. Our team approaches each extraction with the goal of preserving comfort, limiting disruption, and creating a clear plan for what comes next. We explain the reasons for removal, the steps involved, and the available options for restoring function and appearance so you can make an informed decision.
Extractions are considered only after careful evaluation and when preserving the natural tooth is not in the patient’s best interest. When a tooth threatens surrounding teeth or overall oral health, removing it can prevent infection, ongoing pain, and complications that would otherwise require more extensive treatment. Every recommendation is tailored to the individual, taking into account medical history, oral condition, and long-term treatment goals.
Our clinicians balance clinical judgment with patient comfort. Before any procedure, we discuss anesthesia and relaxation options, review any relevant medical concerns, and outline a recovery plan. Clear communication helps reduce anxiety and sets expectations so patients can focus on healing.
Persisting primary (baby) teeth that interfere with normal development
Normally, baby teeth fall out to make room for permanent teeth. Occasionally a primary tooth remains anchored too long — its roots may not resorb properly or it may fuse to the jawbone. When a retained baby tooth obstructs the eruption of a permanent tooth or threatens alignment, timely removal can protect a child’s developing bite and avoid more complex orthodontic issues later.
A permanent tooth with irreparable decay or structural loss
Decay begins at the enamel and, if left untreated, progresses toward the tooth’s inner layers. Once a cavity has destroyed too much structure or spread to the root in a way that cannot be reliably restored, extraction becomes the most prudent option to remove infected tissue and prevent further spread to adjacent teeth or bone.
Severe fractures or complex tooth damage
Teeth can sustain fractures in several patterns; some are repairable, while others compromise the tooth’s integrity beyond restoration. When the damage extends beneath the gumline or into the root such that a sound, lasting repair is unlikely, removing the tooth can be the safest, most predictable route to resolving pain and preventing infection.
Advanced periodontal disease affecting supporting tissues
Gum disease can steadily erode the bone and soft tissue that anchor teeth. In advanced cases where the supporting structures are irreversibly compromised, extraction may be required to stop the spread of infection and protect neighboring teeth. Addressing the disease process—through cleanings, periodontal therapy, and improved home care—is an important part of treatment before and after extractions.
Problematic or impacted wisdom teeth
Third molars frequently lack adequate space to erupt and can become impacted, decayed, or a source of crowding and infection. Removing troublesome wisdom teeth often prevents recurring pain, damage to adjacent teeth, and other complications. The timing and approach depend on the individual’s development and clinical findings.
Extractions as part of orthodontic planning
When the jaws don’t have enough room for all the permanent teeth, carefully selected extractions can create the space needed to align the bite and achieve a stable, functional result. Any extraction performed for orthodontic reasons is coordinated closely with the orthodontic plan to optimize long-term outcomes.
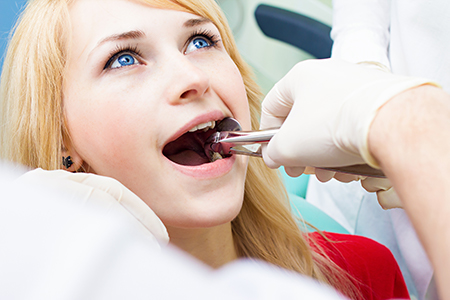
Before a single instrument is used, your provider will review your health history, medications, and any concerns that could affect treatment. Understanding your overall health helps determine whether pre-procedure measures — such as antibiotics, medication adjustments, or medical clearance — are appropriate. We encourage patients to share any recent changes in health so we can tailor care safely.
Diagnostic imaging, most commonly a digital radiograph, clarifies root shape, bone levels, and nearby structures. This imaging helps the clinician decide whether a tooth can be removed with a straightforward approach or will require a surgical technique. We’ll explain the chosen approach so you know what to expect during the visit.
Comfort is prioritized throughout. Local anesthesia effectively numbs the area, and for patients who prefer additional relaxation we discuss sedation options. With clear anesthesia and effective communication, the procedure itself is typically brief; surgical cases can take longer and may be referred to a specialist when appropriate for complex anatomy or impacted teeth.
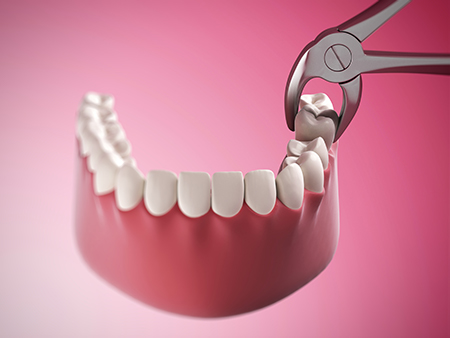
Simple extractions are performed on teeth that are visible and easily accessed in the mouth. After numbing the area, the clinician loosens periodontal attachments and removes the tooth using specialized forceps. For many patients, a simple extraction is quick and healing is straightforward when post-op instructions are followed.
Surgical extractions are used when a tooth is broken at the gumline, has an unusual root shape, is ankylosed, or is impacted beneath the bone. This procedure may require a small incision in the soft tissue and selective removal of bone to gain access. Because it is more involved, surgical extractions are handled with additional planning and sometimes in collaboration with an oral surgeon to ensure the safest outcome.
We will review anesthesia choices, suturing expectations, and recovery timelines for either approach so you can plan transportation, rest, and any assistance you may need after the visit.
Careful aftercare is the most important factor in minimizing discomfort and supporting recovery. We provide tailored post-operative instructions that cover bleeding control, swelling management, pain relief, and when to resume normal activities. While many patients follow a routine recovery pattern, the specifics may vary based on the type of extraction and personal health considerations.
Maintaining the initial gauze dressing and applying gentle pressure helps the socket form a stable blood clot, which is essential to healing. Avoiding behaviors that might disturb that clot—such as rinsing vigorously, using a straw, or smoking—reduces the risk of complications like a dry socket. Proper hydration and a soft-food diet for the first 24–48 hours support comfort and recovery.
If sutures are placed, a follow-up visit may be scheduled to check healing and remove stitches if needed. We also discuss when tooth replacement should be considered so you have time to weigh options and plan for long-term function and aesthetics.
Maintain gentle pressure with gauze
Right after the extraction, bite on the provided gauze to help stop bleeding. Replace the gauze as directed and keep pressure for the recommended intervals. Minor oozing can continue for up to 24 hours, but contact the office if bleeding is heavy or persistent.
Protect numb tissues
Until sensation returns, take care not to accidentally bite your lips, cheeks, or tongue. Numbness can hide small injuries that are otherwise easy to avoid.
Take medications as instructed
Antibiotics:
If an antibiotic is prescribed, take the full course exactly as directed to prevent or control infection.
Pain relief:
Use over-the-counter or prescription pain relievers as recommended to stay ahead of discomfort. Follow dosing instructions carefully and discuss any concerns about medications with your provider.
Protect the clot for healing
Avoid rinsing forcefully, spitting, or using straws for the first day or two. These actions can dislodge the clot and delay healing.
Manage swelling with ice
Apply an ice pack to the cheek in short intervals during the first 24 hours to reduce swelling. After the first day, warm compresses can help if stiffness persists.
Avoid tobacco
Smoking and other tobacco use interfere with clot formation and tissue healing. It’s best to avoid these for at least a week after extraction when possible.
Choose gentle foods and stay hydrated
Start with cool or room-temperature soft foods and liquids. Avoid hot, spicy, or crunchy items until healing progresses. Drinking plenty of fluids supports recovery.
Maintain careful oral hygiene
Brush the rest of your teeth gently and avoid disturbing the surgical site. After the initial 24–48 hours, a mild saltwater rinse can help keep the area clean—use it gently to avoid dislodging the clot.
Keep follow-up appointments
Return visits allow us to monitor healing, remove sutures if necessary, and move forward with any planned restorative care. Follow-up is an important part of a successful outcome.
If you notice increasing pain, swelling, persistent bleeding, fever, or any other concerning symptoms, contact the office so we can evaluate and provide prompt care.
Losing a tooth creates both functional and cosmetic considerations. Once the socket has healed, there are reliable options to replace the missing tooth and restore chewing ability and appearance. Common solutions include removable dentures, fixed dental bridges, and dental implants, each with distinct benefits depending on the situation.
A removable prosthesis can replace one or several teeth and can be a conservative, adaptable choice. Bridges use adjacent teeth for support and restore a natural look and feel when neighboring teeth are healthy. Dental implants provide a long-term solution that replaces the tooth root as well as the crown, preserving bone and offering excellent function. We’ll review the most appropriate replacement options based on your goals, oral health, and timeline for treatment.
Coordinating extraction and replacement planning from the start helps streamline care and improves long-term results. If immediate replacement is not recommended at the time of extraction, we’ll outline a clear sequence for staged treatment so you know what to expect.
Tooth extractions are a common and well-understood part of dental care when they are needed to protect oral and overall health. With careful assessment, clear communication, and personalized aftercare, most patients experience predictable healing and good outcomes. The team at Granby Dental Center prioritizes your comfort and recovery, and we work with you to plan any necessary restorative steps following an extraction.
If you have questions about whether an extraction is the right option, what to expect during the appointment, or how best to care for yourself afterward, please contact us for more information. We’re here to help you make the choice that’s best for your health and peace of mind.

Extraction is recommended when preserving a natural tooth would cause ongoing harm or when restorative treatments are unlikely to succeed. Common reasons include severe decay that reaches the root, structural fractures that extend below the gumline, advanced periodontal disease that has compromised supporting bone, and teeth that obstruct proper eruption. Removing a problematic tooth can stop the spread of infection and protect adjacent teeth and oral tissues.
Decisions about extraction are made after a careful evaluation of medical history, diagnostic imaging, and treatment goals. The clinician will explain alternatives and why extraction may be the safest, most predictable option in a specific case. The team at Granby Dental Center tailors recommendations to each patient’s needs and long-term oral health plan.
A simple extraction refers to removing a tooth that is visible and can be accessed easily with forceps after numbing the area. The clinician loosens periodontal attachments and removes the tooth in a controlled manner, and this approach usually involves minimal tissue disruption. Recovery from a simple extraction is typically straightforward when post-operative instructions are followed.
Surgical extractions are used when a tooth is broken at the gumline, impacted, ankylosed, or has an unusual root shape that prevents easy removal. This procedure may involve a small incision in the gum, selective bone removal, and suturing to assist healing. Surgical cases require additional planning and sometimes collaboration with an oral surgeon to ensure a safe outcome.
Preparation begins with a thorough review of your health history, current medications, and any medical conditions that could affect treatment. Diagnostic imaging clarifies root anatomy and nearby structures and helps the clinician choose the safest approach. If you take medications that affect bleeding or immune response, your provider will advise whether adjustments or medical clearance are needed.
If sedation is planned, you may be asked to fast for a period and to arrange transportation home after the procedure. Wear comfortable clothing and bring a list of medications and any questions you have about anesthesia or recovery. Following the pre-procedure instructions provided by the office helps minimize risks and ensures a smoother appointment.
Local anesthesia is used routinely to numb the extraction site and provide effective pain control during the procedure. For patients who need additional relaxation, options such as nitrous oxide (laughing gas), oral sedatives, or intravenous (IV) sedation may be available depending on medical suitability and the complexity of the case. The choice of anesthesia is guided by your comfort level, medical history, and the nature of the extraction.
Your clinician will discuss benefits, risks, and recovery expectations for each option and obtain informed consent before proceeding. Some sedative options require a responsible adult to drive you home and a brief period of post-procedure monitoring. Clear communication about past experiences with anesthesia and any health concerns helps the team select the safest plan.
Before treatment begins, your provider will confirm your medical history, review imaging, and explain the chosen approach to the extraction. Local anesthesia is administered to numb the area, and additional sedation is provided if agreed upon. For a simple extraction the clinician loosens attachments and removes the tooth, while surgical cases may involve making a small incision and removing bone to access the tooth.
During the procedure the team monitors your comfort and communicates each step so you know what to expect. If sutures are needed they will be placed to support healing and may require removal at a follow-up visit. After the extraction you will receive clear post-operative instructions about bleeding control, pain management, and activity restrictions.
Initial recovery typically covers the first 24 to 72 hours, when swelling and discomfort are most noticeable and should gradually improve. A stable blood clot forming in the socket is essential for healing, so patients are advised to avoid actions that might dislodge it. Most routine activities can be resumed within a few days, although heavy exertion should be postponed until healing has advanced.
Complete bone remodeling and soft-tissue maturation occur over several weeks to months, and follow-up visits allow the clinician to monitor progress. Pain and swelling that steadily decrease are normal, but increasing pain, persistent heavy bleeding, fever, or unusual drainage should prompt a call to the office. Adhering to aftercare guidelines speeds recovery and reduces the risk of complications.
Complications after extraction can include dry socket, infection, prolonged bleeding, and in rare cases nerve irritation or injury. Dry socket typically presents as intense localized pain several days after extraction and may be treated with medicated dressings, pain control, and supportive care. Infections are usually managed with appropriate antibiotics and drainage if needed, guided by clinical findings.
Your provider will review warning signs to watch for and when to seek prompt attention, such as increasing pain, fever, swelling that worsens, or persistent bleeding. Most complications are manageable when identified early, and timely follow-up helps prevent progression. Clear post-operative instructions and good oral hygiene reduce the likelihood of problems.
Timing for tooth replacement depends on the extraction site, overall oral health, and treatment goals; some situations allow for immediate replacement while others require healing first. Common replacement options include removable partial dentures, fixed bridges, and dental implants, each offering different benefits for function, esthetics, and long-term oral health. The clinician will discuss which option best fits your needs and timeline.
Dental implants restore the tooth root as well as the crown and are often the preferred long-term solution for suitable candidates, while bridges and removable prostheses may be appropriate in other clinical situations. If bone volume is insufficient, staged treatments such as bone grafting may be recommended to prepare the site for an implant. Your care team will outline a coordinated treatment plan so you understand the sequence and expected outcomes.
Wisdom teeth are evaluated with a clinical exam and imaging to determine eruption status, angulation, and effect on adjacent teeth and tissues. Removal is recommended for teeth that are impacted, causing infection, contributing to crowding, or associated with cysts or decay that cannot be managed conservatively. The decision to remove wisdom teeth balances current symptoms, future risk, and the patient’s overall oral health.
Timing often falls in the late teen years to early adulthood when removal can be more predictable, but each case is individualized. Surgical extractions for impacted third molars may require more extensive planning and, in some cases, referral to an oral surgeon. Your provider will explain the rationale for removal, the expected procedure, and the recovery process so you can make an informed choice.
Extractions for children often focus on retained primary teeth that impede eruption of permanent teeth, severe decay that cannot be restored, or trauma that compromises a tooth. Pediatric care emphasizes behavior management, minimally invasive techniques when possible, and close coordination with parents or guardians. In many pediatric cases the clinician will consider growth and development when planning treatment to minimize long-term impact on the bite.
When extractions are part of orthodontic planning, collaboration with an orthodontist helps ensure space is created in a way that supports proper alignment. Sedation choices and post-operative instructions are tailored for younger patients to ensure safety and comfort. Ongoing monitoring of eruption and development informs any further restorative or orthodontic steps as the child grows.

Scheduling your next visit to Granby Dental Center is quick and hassle-free. Whether you have a specific question about our services or just need to easily book a routine cleaning, our professional staff is here to provide clear answers and simple solutions.
We’ve made it easier than ever to get in touch: give us a call or use our quick online form. Don't put your oral health on the back burner, connect with us today and let us handle the details while you focus on your smile.