At Granby Dental Center, we help patients restore healthy, attractive smiles after tooth loss. Missing teeth change more than appearance — they alter how you chew, speak, and how the rest of your teeth settle in the mouth. This page explains how dental bridges work, why they remain a reliable choice for many people, and what you can expect when considering a bridge as part of a long-term treatment plan.
When a tooth is lost, the space it leaves behind disrupts the balance of forces inside the mouth. Adjacent teeth can tip or drift into the gap over time, which changes your bite and can create new areas that trap food and plaque. Those changes raise the risk of decay, gum disease, and additional tooth loss if left unaddressed.
Teeth in the opposite arch may also move or extrude when they no longer meet an opposing partner, which further compromises chewing efficiency and comfort. Altered chewing patterns can overload remaining teeth, increasing wear and sensitivity and sometimes causing jaw joint (TMJ) symptoms.
Beyond function, tooth loss affects how you feel about your smile and how you communicate. A properly planned tooth replacement restores contact between teeth, preserves alignment, and helps maintain the normal contours of the jaw and face by preventing gradual bone and tissue changes.
Today’s dentistry offers several strategies to replace missing teeth, from removable appliances to fixed restorations anchored to teeth or implants. Each approach has clinical strengths, and the right choice depends on the number of missing teeth, the health of surrounding teeth and bone, and the patient’s goals for durability and appearance.
Fixed bridges have been refined with modern materials and techniques to deliver attractive, long-lasting results when the adjacent teeth provide reliable support or when implants are used as anchors. They offer a predictable, non-removable solution that restores normal function and makes daily oral care straightforward.
Because every patient’s mouth is unique, treatment planning typically involves imaging and a careful evaluation of oral health, chewing dynamics, and long-term maintenance needs. A bridge is often recommended when it can preserve adjacent tooth structure and provide stable occlusion without compromising other aspects of dental health.
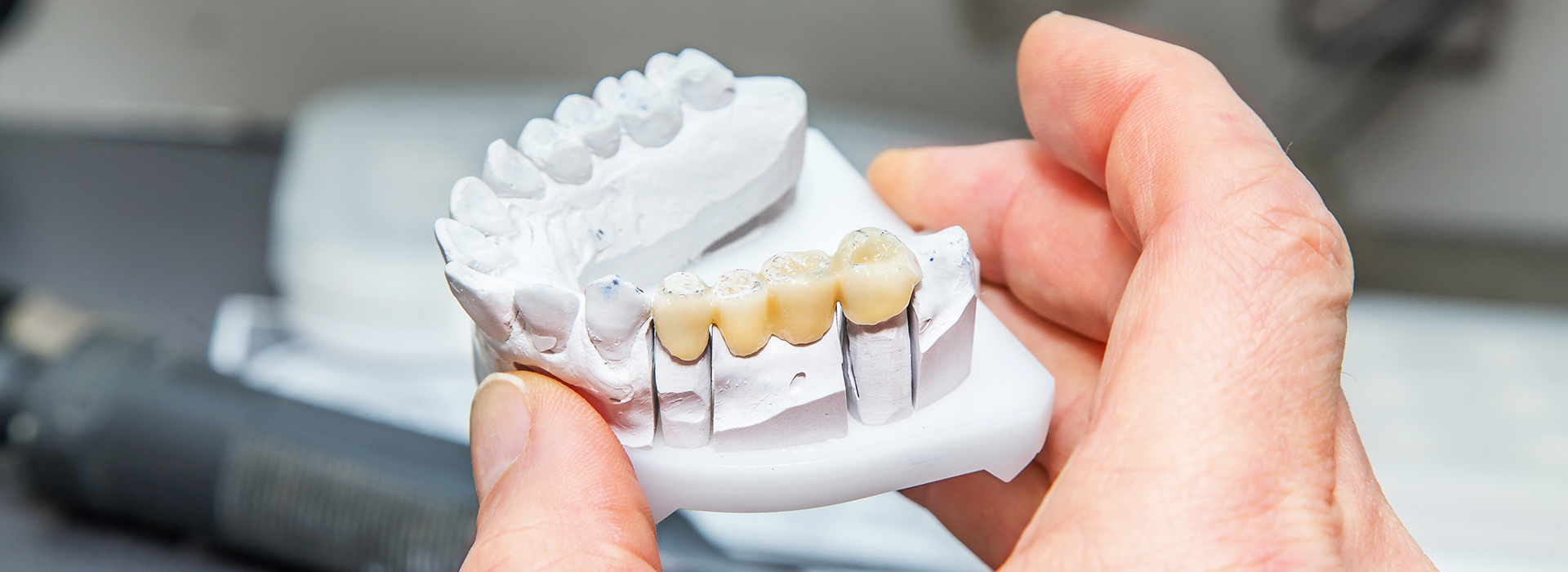
A dental bridge replaces missing teeth with artificial crowns (pontics) that are held in place by support elements on either side. In a tooth-supported bridge, those supports are crowns placed over natural teeth that are prepared to accept the restoration. In an implant-supported bridge, dental implants serve as the foundations, eliminating the need to alter healthy neighboring teeth.
Materials used for bridges today combine strength with lifelike aesthetics. Porcelain, porcelain fused to metal, and high-strength ceramics such as zirconia are commonly selected to match surrounding teeth in color and translucency while withstanding the forces of chewing. The choice of material depends on the location of the bridge, the bite, and cosmetic expectations.
Besides restoring appearance and chewing ability, a well-designed bridge helps maintain tooth position and evenly distributes bite forces, which protects remaining natural teeth and reduces the chance of future complications. With routine care and periodic professional evaluations, bridges can perform reliably for many years.
Traditional bridges anchor to teeth adjacent to the gap and require those teeth to be prepared for crowns. This option is efficient when the supporting teeth are healthy but already need crowns or are strong enough to serve as stable abutments. Preparation alters the tooth structure, so the condition and prognosis of the abutment teeth are important factors in decision-making.
Implant-supported bridges bypass natural teeth by using titanium posts that integrate with the jawbone as anchors. Because implants function like tooth roots, they provide excellent support without involving neighboring teeth. This approach preserves adjacent tooth structure and can also help maintain the volume and shape of the jawbone over time.
Each method has clinical trade-offs related to surgical requirements, the need for sufficient bone, and treatment timeline. A thorough evaluation, including imaging and discussion of goals, helps determine which bridge type aligns best with a patient’s oral health and lifestyle while minimizing future maintenance needs.
Before a bridge is made, the mouth must be healthy and free of active disease. That means managing any gum inflammation, treating cavities, and addressing problems that could compromise the longevity of the restoration. If bone support is inadequate for an implant, bone-grafting procedures can sometimes rebuild the foundation needed for implant placement.
The steps for a traditional fixed bridge commonly include tooth preparation, impressions or digital scans, placement of a temporary restoration, and final cementation once the laboratory-made bridge is ready. Patients can expect short-term sensitivity and adjustment to the temporary, followed by refinement of fit and bite when the permanent bridge is placed.
When implants are part of the plan, treatment begins with surgical placement of the implant posts under sterile, controlled conditions. Healing time is required to allow the implants to integrate with the bone; once this process is complete, abutments and the final prosthesis are attached. In some situations a temporary tooth is provided for immediate appearance during healing.
After any bridge is placed, regular checkups and a daily oral hygiene routine are vital. Bridges require the same attention as natural teeth: brushing, flossing in the areas around and beneath the pontic, and periodic professional cleanings to monitor fit and health. Proactive maintenance helps maximize the life of the restoration and the health of the supporting tissues.
We aim to provide clear, individualized guidance when patients are weighing tooth-replacement options. If you’d like to learn more about whether a dental bridge is a good fit for your smile, please contact us for additional information and to schedule an evaluation with our team at Granby Dental Center.

A dental bridge is a fixed prosthetic used to replace one or more missing teeth by spanning the gap between adjacent teeth or implants. It typically consists of one or more artificial teeth, called pontics, connected to support crowns or implant abutments. Bridges are designed to restore normal chewing function, maintain proper tooth alignment, and improve the appearance of the smile.
Bridges can be supported by natural teeth that are prepared to receive crowns or by dental implants that act as independent anchors. The choice of support depends on the health of the adjacent teeth, the amount of available bone, and the patient’s long-term goals for durability and oral health. A well-planned bridge becomes a non-removable part of the mouth that simplifies daily care compared with many removable appliances.
Good candidates for a dental bridge are patients who have one or more missing teeth and generally healthy surrounding teeth and gums. Candidates should be free of uncontrolled gum disease or active decay, because these conditions can compromise the longevity of the restoration. Sufficient bone and favorable tooth positions also contribute to predictable outcomes for both tooth-supported and implant-supported bridges.
During an evaluation, the dentist will review medical and dental history, examine the mouth, and often obtain imaging to assess bone levels and tooth structure. If problems such as gum inflammation or decay are present, those issues are managed before bridge placement to improve long-term success. The final recommendation considers function, esthetics, and the patient’s preferences for treatment and maintenance.
A tooth-supported bridge uses crowns on natural teeth adjacent to the missing tooth or teeth as anchors, while an implant-supported bridge is secured to titanium implants placed in the jawbone. Tooth-supported bridges require preparation of the abutment teeth to accommodate crowns, which can be appropriate when those teeth already need restoration or are strong enough to serve as reliable supports. Implant-supported bridges avoid altering adjacent healthy teeth because the implants function like artificial roots.
Implant-supported bridges can also help preserve bone in the area of the missing teeth because implants transmit functional load to the jawbone. The choice between these options depends on factors such as bone availability, overall oral health, surgical considerations, and the patient’s timeline for treatment. A comprehensive consultation and imaging help determine which approach best balances preservation of tooth structure, function, and esthetics.
Modern bridges are made from a variety of materials chosen for strength, esthetics, and the location of the restoration. Porcelain fused to metal combines a durable metal substructure with a tooth-colored porcelain surface for improved appearance and strength in posterior areas. All-ceramic materials, including high-strength zirconia and layered ceramics, offer excellent esthetics and are often used in visible areas to achieve a natural translucency and color match.
The material selected will depend on bite forces, the span of the bridge, and the patient’s cosmetic expectations. In some cases, full-contour zirconia is chosen for its durability and fracture resistance, particularly for long-span or posterior bridges. The dentist will discuss material options and make a recommendation based on clinical needs and long-term performance considerations.
Treatment for a traditional tooth-supported bridge usually begins with a thorough exam, treatment of any active disease, and preparation of the abutment teeth. The prepared teeth are shaped to receive crowns, impressions or digital scans are taken, and a temporary bridge is placed to protect the area while the laboratory fabricates the final restoration. At the placement appointment, the temporary is removed, fit and bite are adjusted, and the final bridge is cemented or bonded.
When implants are part of the plan, treatment begins with surgical placement of the implant posts followed by a healing period to allow osseointegration with the bone. After integration, abutments and the final prosthesis are attached, and any necessary adjustments are made to optimize fit and function. Throughout both paths, careful diagnostics and stepwise care reduce complications and support predictable long-term results.
Daily hygiene for a dental bridge includes thorough brushing and cleaning beneath the pontic to remove plaque and prevent gum inflammation around the supports. Flossing under a bridge often requires special tools such as floss threaders, interdental brushes, or water irrigation to clean the space between the pontic and gum effectively. Maintaining excellent oral hygiene helps protect the supporting teeth and tissues from decay and periodontal disease.
In addition to home care, regular professional cleanings and dental exams are important to monitor the bridge’s fit and the health of surrounding structures. Your dentist or hygienist will check for signs of wear, bite changes, or tissue problems and recommend interventions if issues arise. Prompt attention to discomfort, looseness, or changes in chewing can prevent small problems from becoming more significant.
Dental bridges are durable restorations that can function well for many years with proper care; many bridges remain serviceable for a decade or longer depending on individual circumstances. Lifespan is influenced by factors such as oral hygiene, the health of the supporting teeth and gums, the material used to fabricate the bridge, and the patient’s bite forces or parafunctional habits like grinding. Regular dental visits and timely maintenance help identify and address problems that could shorten a bridge’s useful life.
Damage to the supporting teeth, recurrent decay, gum disease, or significant changes in bite can compromise a bridge and lead to the need for repair or replacement. For implant-supported bridges, successful osseointegration and good bone health are critical to long-term stability. Your dentist will discuss realistic expectations and a maintenance plan tailored to your situation during the treatment planning process.
Common risks include decay or fracture of the abutment teeth, gum inflammation, and loosening of the restoration if supporting structures deteriorate. Tooth-supported bridges require preparation of adjacent teeth, which can increase the risk of future problems with those teeth if underlying issues are present. Implant-supported bridges carry surgical risks such as infection or inadequate bone support, though careful planning reduces these chances.
Other potential complications include changes in bite or discomfort that require adjustment, wear of opposing teeth, and difficulty cleaning around the restoration if access is limited. A thorough evaluation before treatment and consistent follow-up care help identify risks early and allow for corrective measures to protect oral health. Patients should report persistent pain, mobility, or changes in fit so the dental team can address them promptly.
A properly designed and fitted bridge typically restores normal chewing ability and has minimal long-term effect on speech. Some patients notice a brief adjustment period as they adapt to the new shape and contours of the restoration, which can slightly alter tongue placement or bite during speech. These changes usually resolve within days to weeks as the patient becomes accustomed to the bridge and any temporary restorations are replaced with the final prosthesis.
Chewing efficiency is often improved because the bridge re-establishes contact between teeth and distributes bite forces more evenly. If speech or chewing problems persist, adjustments to the shape, height, or contact points of the bridge can often correct the issue. Communicating concerns to the dental team early ensures timely refinements and a comfortable functional result.
Yes, by filling the space left by a missing tooth, a dental bridge helps maintain proper tooth alignment and prevents adjacent teeth from drifting into the gap. This preservation of occlusion supports balanced chewing forces and reduces the likelihood of bite changes that can affect other teeth and the temporomandibular joint. Replacing missing teeth also helps maintain facial contours by supporting the soft tissues that can otherwise gradually change when multiple teeth are lost.
It is important to note that while tooth-supported bridges restore function and alignment, they do not replace the tooth root; therefore, they do not prevent bone resorption at the site of the missing root in the same way that implants can. When maintaining bone volume is a priority, an implant-supported solution may be discussed as an alternative that more directly preserves the underlying jaw structure. During evaluation, the dentist will review how each option supports long-term oral health and structural needs.

Scheduling your next visit to Granby Dental Center is quick and hassle-free. Whether you have a specific question about our services or just need to easily book a routine cleaning, our professional staff is here to provide clear answers and simple solutions.
We’ve made it easier than ever to get in touch: give us a call or use our quick online form. Don't put your oral health on the back burner, connect with us today and let us handle the details while you focus on your smile.